The main reason many RHTP initiatives will fall short of achieving the outcomes expected by CMS is not technology — it is the unmanaged resistance to change by clinicians, by staff, by administrators, and by patients. Sustainable transformation requires a deliberate, structured approach to moving the hearts, minds, and habits of every person involved.
Over the past four articles, we have built a complete picture of what it actually takes to lead sustainable change in rural healthcare.
The Switch framework gave us the psychology: engage the rational mind with clear direction, motivate the emotional side with feeling and identity, and shape the environment to make the right behavior easier than the old one. Nine tactics for moving people, not just processes.
The ADKAR® model gave us the sequence: build Awareness, create Desire, supply Knowledge, develop Ability, and reinforce the change until it holds — and use the model as a diagnostic when something stalls. Five conditions, no shortcuts.
Covey’s 7 Habits gave us the character and the practice: three habits of preparation that set the foundation, three habits of engagement that cultivate and sustain desire, and one habit of renewal that makes everything last.
Together, those three frameworks offer 21 distinct approaches to the human side of change. They are powerful. Yet they are not sufficient on their own.
Because change doesn’t manage itself. Even the most psychologically sophisticated, sequentially sound, and habitually disciplined change initiative will drift without deliberate structural support.
That support comes from three disciplines drawn from the Project Management toolkit:
-
Stakeholder Management
-
Communications Management
-
Risk Management
These are not bureaucratic formalities. They are the scaffolding that holds everything else together — especially in the complex, high-stakes environment of RHTP implementation.
Stakeholder Management: Change Happens Through People
Every project has stakeholders. But in change management, understanding who your stakeholders are — and what they need — is not a preliminary task. It is the task.
A stakeholder is any individual who holds a stake in the success of the initiative: someone who will be rewarded by its success, impacted by its outcomes, or whose support or resistance will meaningfully affect the initiative’s trajectory.
In an RHTP service launch implementation, that list is longer than most leaders initially assume. It includes clinicians, nurses, care coordinators, front desk staff, administrators, IT personnel, patients, community members, board members, state health officials, and payers.
Not all stakeholders are equal in their influence or their interest — and treating them as if they were is one of the most common and costly mistakes in change management.
A practical tool for navigating this reality is the Stakeholder Influence/Interest Matrix: a simple framework that plots stakeholders on two axes — level of influence (high to low) and level of interest (high to low) — producing four distinct engagement strategies.
Manage Closely — high influence, high interest: your clinical champions, CMO, CNO, and key department leads. These are your essential partners. Engage them early, engage them often, and wherever possible, co-design the change with them. Their buy-in is not optional.
Keep Satisfied — high influence, low interest: your CEO, board members, and state health officials. They don’t need every operational detail, but they must never be surprised by a significant development. Keep them informed at key milestones and ensure they can speak confidently about the initiative when asked.
Keep Informed — low influence, high interest: front desk staff, care coordinators, and patients. They are directly affected by the change and care deeply about what it means for them. Regular, clear communication builds trust and reduces the anxiety that fuels resistance.
Monitor — low influence, low interest: peripheral stakeholders who need occasional awareness but not active engagement.
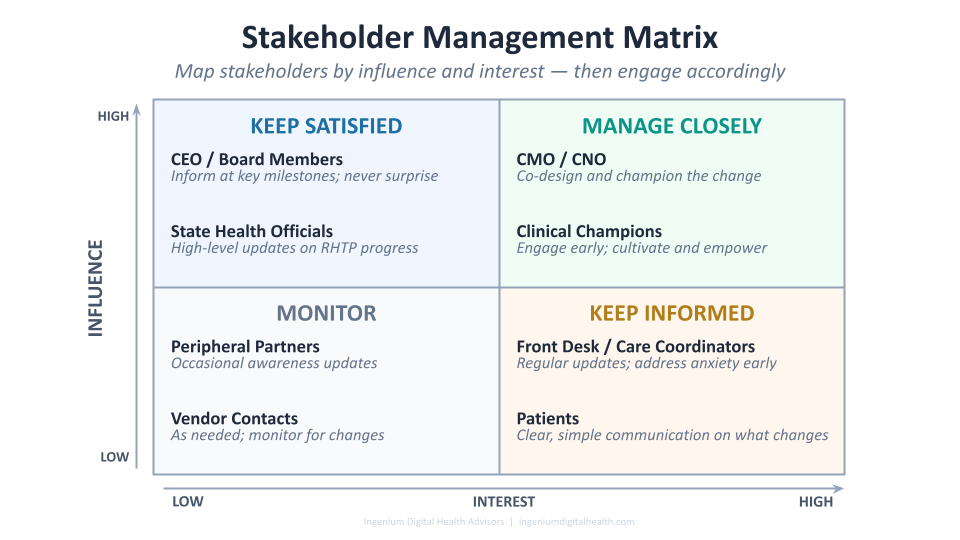


The matrix is a starting point, not a permanent assignment. Stakeholders move — a front desk staff member who becomes an early adopter may gain influence quickly. A senior clinician who was initially neutral may become a vocal resistor. Stakeholder management is a living practice, not a one-time exercise.
Connecting back to our frameworks: stakeholder management is where ADKAR’s Awareness and Desire meet the 7 Habits’ Habit 3 (Put First Things First) and Habit 4 (Think Win-Win). Knowing who needs what, and in what sequence, is the foundation of every other change management effort.
Communications Management: Intentional, Personalized, Sustained
Change does not communicate itself. And yet communication is the element most frequently left to chance in implementation planning — a kickoff email here, an all-staff meeting there, and an assumption that word will travel.
It won’t. Not reliably. Not in ways that build Awareness, create Desire, or sustain Reinforcement.
Effective communications management begins with a communications plan — a deliberate document that answers four questions for each stakeholder group:
-
What do they need to know?
-
When do they need to know it?
-
How do they prefer to receive information?
-
Who is responsible for delivering it?
That third question — how do they prefer to receive information — is the one most implementation teams skip. And it is often the difference between a message that lands and one that is ignored.
Every stakeholder has different communication preferences. Some want a formal status report. Others want a brief personal email. Some respond best to a dashboard they can check on their own schedule. Others need a phone call. Some are reachable by text; others by including updates in an existing meeting or workflow they already attend. Taking the time — early in the project, before the change begins — to ask each key stakeholder how they want to be kept informed is not a courtesy. It is a strategic investment that dramatically increases the likelihood that your communications actually reach the people who need them.
A well-designed communications plan also maps message content to the ADKAR sequence. Early communications build Awareness — the human case for why the change is needed, told in terms that resonate with each stakeholder group. As the project progresses, communications shift to cultivating Desire — speaking to WIIFM, sharing early wins, celebrating bright spots. After launch, communications focus on Reinforcement — performance data, peer recognition, ongoing updates that signal the change is real, valued, and here to stay.
Communications management is also where Covey’s Habit 2 (Begin with the End in Mind) and Habit 5 (Seek First to Understand) come to life operationally. The destination must be communicated repeatedly and emotionally. And the preferences of each stakeholder must be understood before the message can be crafted to reach them.
Risk Management: Proactive, Not Reactive
By the time a risk becomes a crisis, the cost of addressing it has multiplied many times over. Risk management is the discipline of identifying what could go wrong — before it does — and putting mitigation strategies in place while there is still time to act.
In RHTP change management, risks are not abstract. They are specific, predictable, and in many cases preventable.
The practical tool is a risk register: a living database that inventories each significant risk, assesses its likelihood and potential impact, assigns ownership, and defines a specific mitigation strategy. It is not a long or complex document. It is a disciplined habit of looking ahead.
Some of the most common — and most consequential — risks in rural telehealth implementation include:
Key person dependency. Your most enthusiastic clinical champion is also one of your most valuable clinicians. What happens if they leave — to a larger system, to burnout, to retirement? In rural healthcare, where staff turnover is chronically high, building a program that depends on one person’s enthusiasm is building on sand. Mitigation: identify and cultivate multiple champions early. Document their knowledge. Build the culture, not just the individual.
Inadequate reinforcement after launch. This is perhaps the most universal risk in healthcare change management — and the most preventable. Without active, ongoing reinforcement, even a well-implemented change will backslide. Old habits reassert themselves quietly. The mitigation is ADKAR’s Reinforcement element made operational: performance measurement, feedback loops, peer recognition, and leadership accountability built into the program from day one — not added after the first signs of drift.
Measuring Activity Instead of Outcomes. The pressure to demonstrate progress — to funders, to boards, to state coordinators — creates a powerful temptation to report what is easy to count: the number of training sessions held, devices deployed, or video visits conducted in the first month. These are input and output measures. They tell you what happened. They do not tell you whether anything changed. A telehealth program that reports 200 video visits in month one but never measures whether patients got better care, whether clinicians sustained adoption, or whether the service is still running in month twelve has mistaken activity for transformation. Mitigation: Build outcome measures into the program from day one — patient satisfaction, clinical quality indicators, sustained utilization, and staff confidence scores — and report on them with the same rigor as the activity metrics.
Workflow integration failure. A telehealth service that runs parallel to existing workflows rather than integrated into them will always feel like extra work. The risk is not just inconvenience — it is that clinicians and staff will route around it whenever possible. Mitigation: invest in current-state process mapping before go-live, and design the new workflow on top of what already exists.
Patient adoption barriers. Rural patients face real and well-documented barriers to telehealth adoption: limited broadband, digital literacy gaps, device access, and cultural preferences for in-person care. A program designed without accounting for these barriers will underperform — not because patients don’t want care, but because the path to accessing it is too difficult. Mitigation: design for the hardest-to-reach patient, not the easiest.
Risk management connects directly to Switch’s Habit 1 (Be Proactive) and to ADKAR’s diagnostic framework. Identifying risks in advance is anticipating where the ADKAR chain is most likely to break — and building the reinforcement before the backsliding begins.
One final and important point: sustainable change is itself a risk criterion. A telehealth program is a project — a unique undertaking with a defined scope, timeline, and budget. But its outcomes must outlive the project. The transformation must continue after the project team disbands, after the grant period ends, after the initial energy fades. Building sustainability into the project objectives — not as an afterthought but as a core success criterion — is the risk management discipline that separates programs that last from programs that were launched.
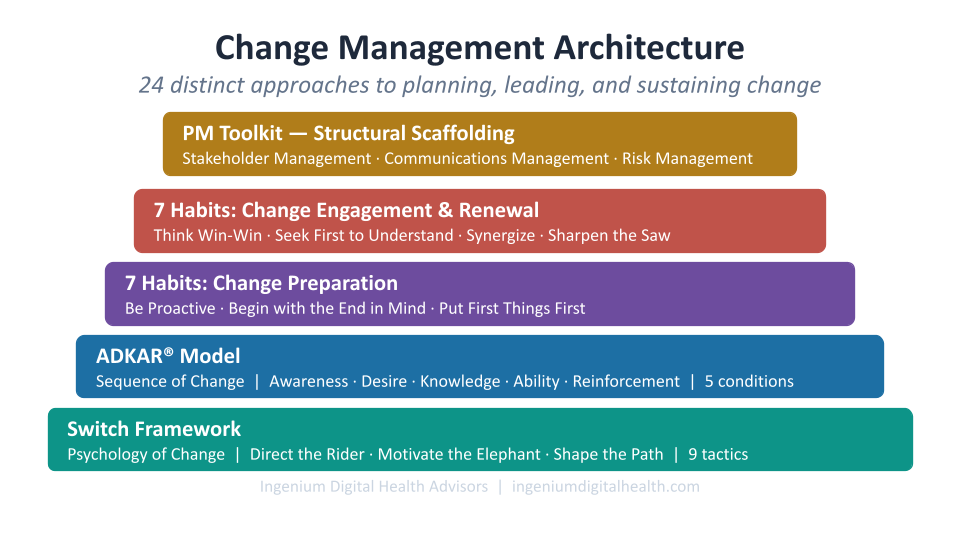


The Complete Change Management Architecture
Five articles. Four frameworks. One mission.
Whether you are reading this as the conclusion of a series or as a standalone guide, here is the complete picture of what conscious, sustainable change management requires for RHTP success:
The Switch Framework (Chip and Dan Heath) gives you nine tactics organized around three forces: Direct the Rider with clear direction and bright spots, Motivate the Elephant with feeling and identity, and Shape the Path to make the right behavior the easy behavior.
The ADKAR® Model (Prosci) gives you five sequential conditions for sustainable change — Awareness, Desire, Knowledge, Ability, and Reinforcement — and a diagnostic framework for identifying exactly which missing element is causing an implementation to stall.
The 7 Habits of Highly Effective People (Stephen Covey) give you seven disciplines organized in three phases: Change Preparation (Be Proactive, Begin with the End in Mind, Put First Things First), Change Engagement (Think Win-Win, Seek First to Understand, Synergize), and Sustaining Change (Sharpen the Saw).
The PM Toolkit gives you three structural disciplines that hold everything together: Stakeholder Management to ensure the right people are engaged in the right ways at the right times, Communications Management to ensure your messages reach stakeholders in the ways they can actually receive them, and Risk Management to ensure you are looking ahead rather than reacting to crises.
Together, these frameworks offer more than 24 distinct approaches to planning, leading, and sustaining change. No single initiative will use all of them. But the change leader who has internalized all of them has something invaluable: the ability to diagnose any change challenge — and reach for exactly the right tool.
The Rural Health Transformation Program is asking rural healthcare organizations to do something genuinely difficult. Not to purchase technology. Not to launch services. But to transform — to achieve the thorough, dramatic change that the word actually requires.
That transformation will not happen by accident. It will not happen through procurement. It will happen through the deliberate, conscious, sustained management of the human side of change.
You now have the toolkit. The question is: To what extent will you use it?
Christian Milaster and his team at Ingenium Digital Health Advisors help rural healthcare organizations build the implementation capability to turn RHTP funding into lasting outcomes. Connect with Christian to explore what proper change management can look like for your RHTP initiative.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.








