A quote from Dr. Charlie Mayo has stayed with me since my years at the Mayo Clinic:
“Today, the only thing that is permanent is change.”
Dr. Mayo’s guidance to the clinic he and his brother started were recorded in 1931. Nearly a century later, they have never been more relevant — and for rural healthcare organizations navigating the Rural Health Transformation Program, they have never carried higher stakes.
Last week, we introduced the Switch framework from Chip and Dan Heath — a model built around three forces that must all be engaged for change to take hold: the rational mind (the Rider), the emotional side (the Elephant), and the environment (the Path) that makes change easy or hard. Nine specific tactics — three for each force — give leaders practical tools for moving people, not just processes.
But knowing how to move people is only part of the equation. The other part is knowing in what sequence — and what goes wrong when you skip a step.
That is where the ADKAR® model comes in.
A Framework Proven in Healthcare
Developed in 1996 by Prosci founder Jeff Hiatt and backed by decades of research, the ADKAR® model has been a cornerstone of organizational change management for over three decades. I was introduced to it 25 years ago during my time at the Mayo Clinic — one of the earliest healthcare organizations to adopt it systematically — and have applied it to telehealth and digital health implementations ever since.
The model is elegant in its simplicity: sustainable change requires five elements, in five specific areas. Leave any one of them out, and the change will not hold. Not because the plan was wrong. Not because the technology failed. But because a critical human need that makes change possible went unmet.
For rural healthcare leaders implementing virtual specialty consults — or any new telehealth service — under RHTP, this framework is not just useful. It is essential.
The Five Elements of ADKAR
ADKAR is an initialism that stands for the five elements: Awareness, Desire, Knowledge, Ability, and Reinforcement.
Raising AWARENESS: The Why
The first element is awareness of the need for the change. It answers the most fundamental question any clinician or staff member will ask, usually silently:
“Why are we doing this?”
For example if you are establishing virtual specialty consults, this means helping everyone understand why the organization is investing in connecting patients to remote specialists via video. The answer is not “because CMS is funding it.” That is an organizational rationale, not a human one. The answer that creates Awareness is this: “Because our patients are driving two hours for a 12-minute neurology appointment — and half of them never even make the trip.”
Awareness is not a memo. It is not an all-staff email. It is a sustained, visible, repeated communication of the human case for change. It’s the “Why”.
Creating DESIRE: The Want
Awareness tells people why the change is happening. Desire determines whether they want to support it.
This is the WIIFM moment — “what’s in it for me?” — and it is the element most commonly underestimated by implementation planners. Desire cannot be mandated. A clinician can be required to attend a training session. They cannot be required to care about what they learned there.
For the example of virtual specialty consults, desire might look different for different stakeholders. For the primary care physician, it may be the satisfaction of finally getting a same-week cardiology opinion on a complex patient. For the care coordinator, it may be eliminating the exhausting logistics of arranging distant referrals. For the patient, it may simply be not having to take a day off work.
Find what matters to each group — and speak directly to that. Without discovering each stakeholder’s WIIFM, the resistance to change will be insurmountable.
In one rural clinic, a primary care physician was unwilling to do telehealth. “It’s not good medicine,” he proclaimed. A year later he bought a beach house — and without missing a beat asked: “Could I do video visits on Fridays from my beach house?”
That’s WIIFM in action.
Supply KNOWLEDGE: The How
Once someone is aware of the need for change and desires to support it, they need to know how. Knowledge is about understanding what is expected: the new workflows, the new policies, the new technology, the new documentation requirements.
For virtual specialty consults, knowledge gaps are substantial and specific. How does a clinician initiate a virtual consult referral? What clinical information needs to be prepared in advance? How does the patient get connected? What happens if the specialist recommends a follow-up? Who documents what, and where?
Without clear answers to these questions, even a willing clinician will hesitate. Knowledge is the bridge between intention and action — and it must be built deliberately, not assumed.
Build ABILITY: The Doing
Knowledge and ability are closely related but critically distinct. Knowledge is knowing what to do. Ability is being able to actually do it — consistently, confidently, under real clinical conditions.
A clinician may know that a virtual specialty consult requires launching a video platform, preparing a clinical summary, and guiding the patient through the connection process. Knowing that is not the same as being able to do it smoothly in the middle of a busy clinic day, with a patient who has never done a video call, while maintaining the clinical focus the encounter requires.
Ability is built through practice, through role-specific training, through the kind of hands-on rehearsal that transforms knowledge into muscle memory. This is why we invest heavily in simulation-based training and structured workflow rehearsals before any new service goes live.
Ensure REINFORCEMENT: The Accountability
The final element — and the one most frequently neglected after launch — is reinforcement. Old habits are remarkably resilient. The comfort of the familiar reasserts itself quietly, gradually, and persistently. Without active reinforcement, even a well-implemented change will backslide.
Reinforcement is not punishment for non-compliance. It is the systematic measurement of performance, the celebration of progress, and the honest identification of gaps — followed by support, not blame.
For virtual specialty consults, this means tracking utilization, measuring clinician and patient satisfaction, monitoring technical success rates, and feeding that information back to the people doing the work in ways that are timely, specific, and actionable.
Reinforcement is what transforms a successful launch into a sustainable program.


ADKAR as a Diagnostic Tool
The most common root cause of failure when launching new services is not a technology problem — it is an unmanaged change problem. Humans are remarkably creative when it comes to resisting change. That creativity is not stubbornness or obstinacy; it is survival instinct. We are wired to protect what is familiar and proven.
To get people to do things differently, you cannot mandate your way there. You need to enroll them — appeal to their hearts and their minds, and make the change feel achievable rather than threatening.
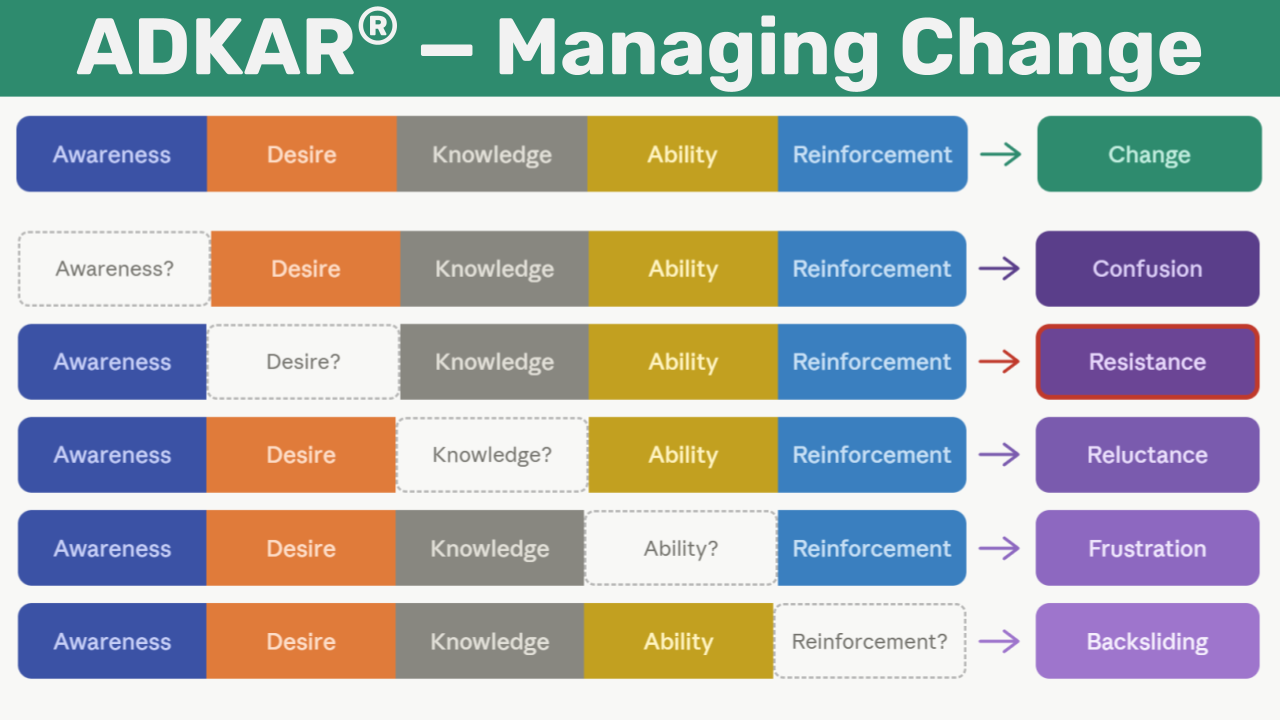
Without deliberate change management, the clinicians, staff, patients, and leaders involved in launching a new service like virtual specialty consults will not simply comply or resist in obvious ways. They will become confused about why the change is happening, resistant to supporting it, reluctant to move forward without more certainty, frustrated by their inability to perform the new skills confidently, or they will backslide into old habits the moment the initial energy fades.
This is precisely where ADKAR® becomes not just a planning tool but a diagnostic one. Each of those five failure modes maps directly to a missing element:
-
Confusion → missing Awareness — people don’t understand why the change is needed
-
Resistance → missing Desire — people don’t want to support it
-
Reluctance → missing Knowledge — people don’t know what’s expected of them
-
Frustration → missing Ability — people can’t execute it confidently
-
Backsliding → missing Reinforcement — the change was never made to stick
When an implementation is struggling, resist the instinct to blame the people or even the technology. Instead, ask: what form of change failure are we encountering? Then identify the element that is missing. The answer will tell you exactly where to intervene — and what kind of support will actually help.
How ADKAR and Switch Work Together
The Switch framework and the ADKAR® model are not competing approaches. They are complementary lenses on the same challenge — and together they are more powerful than either alone.
Switch tells you how to move people: engage the rational mind with clear direction, motivate the emotional side with feeling and identity, and shape the environment to make the right behavior easier. It is a framework of tactics.
ADKAR tells you what people need, in sequence, for change to be sustainable. It is a framework of conditions.
The mapping between them is natural:
Awareness is built through Switch’s “Point to the Destination” and “Find the Feeling” — giving people both the rational case and the emotional resonance for why change is needed.
Desire is cultivated through “Grow Your People” and “Find the Feeling” — connecting the change to identity and to what genuinely matters to each stakeholder.
Knowledge is delivered through “Script the Critical Moves” — making the expected behaviors so specific and clear that uncertainty has nowhere to hide.
Ability is developed through “Build Habits” and “Shrink the Change” — practicing the new behaviors in bounded, low-stakes settings until they become routine.
Reinforcement is sustained through “Rally the Herd” and “Tweak the Environment” — using peer influence and structural support to make the new way of working the default, not the exception.
Used together, Switch and ADKAR give rural health leaders both the tactical playbook and the diagnostic framework to implement RHTP initiatives that don’t just launch — they last.
Next in the series: the structural mechanics of change — stakeholder management, project discipline, and performance reinforcement — and how they hold everything together over the long run.
What’s the biggest change management challenge your organization is facing right now? Reply and let me know.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.








