With millions of dollars in Rural Health Transformation Program (RHTP) funding now flowing to organizations in all 50 states, rural hospitals, critical access hospitals, and health systems face a pivotal question:
What telehealth services should we actually launch?
For many organizations, the instinct is to start with and expand the use of video visits. And that’s a reasonable instinct — but it’s also an incomplete one. Telehealth is a much broader toolkit than a video call, and RHTP represents a unique opportunity to thoughtfully and strategically expand access and improve outcomes through telehealth modalities beyond video.
One challenge is that many rural residents can’t access even a basic video visit. They may lack the technology, the broadband connection, or the digital literacy to connect on a smartphone or computer. And for those who can connect, a scheduled visit alone rarely addresses the full scope of what rural patients need — particularly those managing chronic conditions.
When thinking about optimizing care delivery in rural America, chronic care management has to be at the center of that conversation. Whether it’s the four classic lifestyle diseases — high blood pressure, high cholesterol, type 2 diabetes, and obesity — or more complex conditions like cancer and severe mental illness, effective treatment requires more than an occasional visit. It requires engagement, continuity, and connection between those visits.
That’s where a broader telehealth strategy becomes not just useful, but essential.
Here are four telehealth solutions that are “delivering care at a distance” that go well beyond the video visit — and that belong in every rural organization’s RHTP planning conversation.
The Power of Secure Messaging
Over the past decade, texting has become the default communication mode for most Americans. It’s asynchronous, low-friction, and deeply familiar. For care teams, it’s also a powerful tool for keeping patients engaged between visits.
Secure, HIPAA-compliant messaging doesn’t require an expensive data plan or a sophisticated smartphone. With informed consent, it can be as simple as a “How are you doing?” or a targeted check-in: “Do you have any questions about your medication?” Small gestures — but they carry enormous weight.
One of the most consistent lessons from the field: patients don’t just want care, they want to feel cared for. The sense of belonging that comes from knowing someone is checking in on them is often as therapeutic as the clinical intervention itself. That kind of human connection is cheap to deliver and nearly impossible to replicate with technology alone — but technology makes it scalable.
A Sense of Belonging through Remote Patient Monitoring
Remote Patient Monitoring (RPM) — tracking blood pressure for hypertension patients, weight for congestive heart failure, glucose for diabetes — is one of RHTP’s most explicitly supported use cases. And for good reason: the clinical value of more frequent monitoring is real.
But the biggest benefit of RPM isn’t the data. It’s the relationship the data enables.
When a monitoring nurse reaches out because a patient’s blood pressure spiked after a high-sodium weekend, that’s a just-in-time teaching moment. When a care team member calls to celebrate two weeks of perfect readings, that’s a signal that someone noticed, someone cares. The monitoring creates the occasion for connection. The connection drives engagement. The engagement drives outcomes.
For rural organizations planning their RHTP telehealth investments, RPM programs deserve serious consideration — not just as clinical tools, but as patient engagement infrastructure.


Community Telehealth Access Points
Not every patient can bring telehealth home. But they may be able to bring themselves to a community hub.
Public telehealth access points — in schools, libraries, community centers, fire stations — solve the triple barrier of transportation, connectivity, and digital literacy simultaneously. A patient who can’t afford broadband and doesn’t own a smartphone can still have a high-quality video visit from a staffed, equipped location in their community.
This model also aligns well with RHTP’s emphasis on keeping care local and building community-based infrastructure. Organizations partnering with schools, libraries, and municipalities to establish access points aren’t just expanding telehealth reach — they’re building the connective tissue of a regional care network.
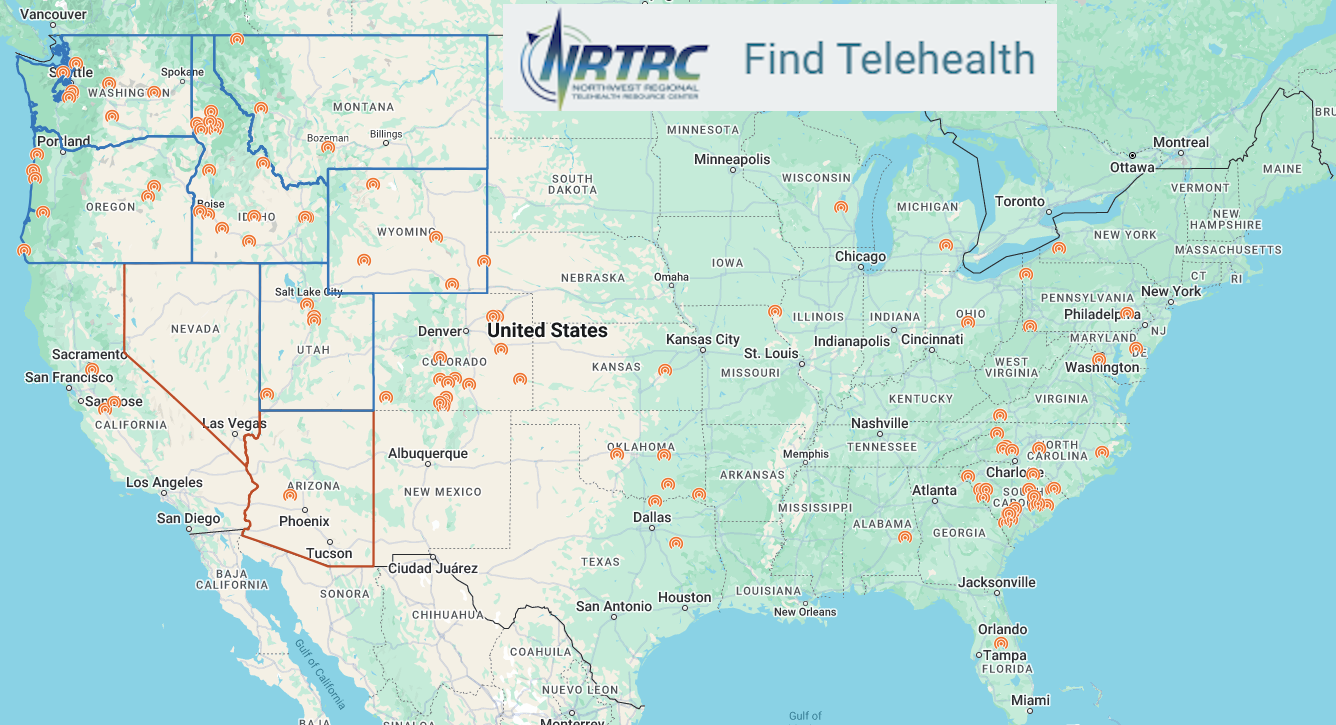
In the Northwest region of the US the Northwest Regional Telehealth Resource Center (NRTRC) has mapped over 100 Telehealth Access Points in a 7 state area.
Community Paramedicine
Community paramedics occupy a unique position in rural health: they’re already in the field, already trusted, and already equipped to respond. What they haven’t always had is the structure and technology to function as an extension of the care team.
When equipped appropriately, community paramedics can conduct home visits for recently discharged patients, connect in real time with supervising clinicians via video, and transmit vital signs or images using specialized exam tools. For high-risk, high-utilizer patients, this model can be transformative — and it maps directly to RHTP goals around reducing avoidable hospitalizations and strengthening community-based care.
Using Technology to Increase the Sense of Belonging
What all four of these solutions share is something that has nothing to do with technology: they make patients feel less alone and accompany them on their health journey.
Isolation and loneliness are critical contributors to poor health outcomes, and in rural America, they’re pervasive. A short trip into town to use a library telehealth kiosk, a home visit from a familiar paramedic, a call from the monitoring nurse — all of these are opportunities to strengthen the human connection at the heart of good care.
As rural hospitals and health systems work through their RHTP planning processes, the question isn’t just “how do we spend this funding?” It’s “what kind of care system are we building for the next generation?” Telehealth — deployed thoughtfully, beyond the video visit — is one of the most powerful answers available.
The technology has never been more capable. The funding (and reimbursement) has never been more available. The question is whether organizations will seize this moment to build something lasting.
What telehealth services are you considering for your RHTP program? We’d love to hear what you’re planning — reach out.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.








