I’ve been fond of using one of the quotes of Don Berwick, the founder and past president of the Institute of Healthcare Improvement (IHI): “Every system is perfectly designed to get the results it gets”. In order to get the results we want (as few direct and as few indirect fatalities from the coronavirus as possible) we need to create systems and leverage processes and tools to thoughtfully manage the unprecedented demand on our healthcare system.
The first design principle of a system that gets us these results focuses on understanding the different affected patient populations and designing different, tailored solutions that are tailored to the differing needs of those populations:
1) The Covid-19 confirmed
1a) Mild or asymptomatic (~80%, 0% mortality)
1b) Severe (~15%, 0% mortality)
1c) Critical (~5%, 50% mortality)
2) The Sick and Injured
2a) sick with mild to severe ailments (ambulatory care)
2b) chronically ill patients (including nursing home residents)
2c) severely sick or injured (requiring hospitalization)
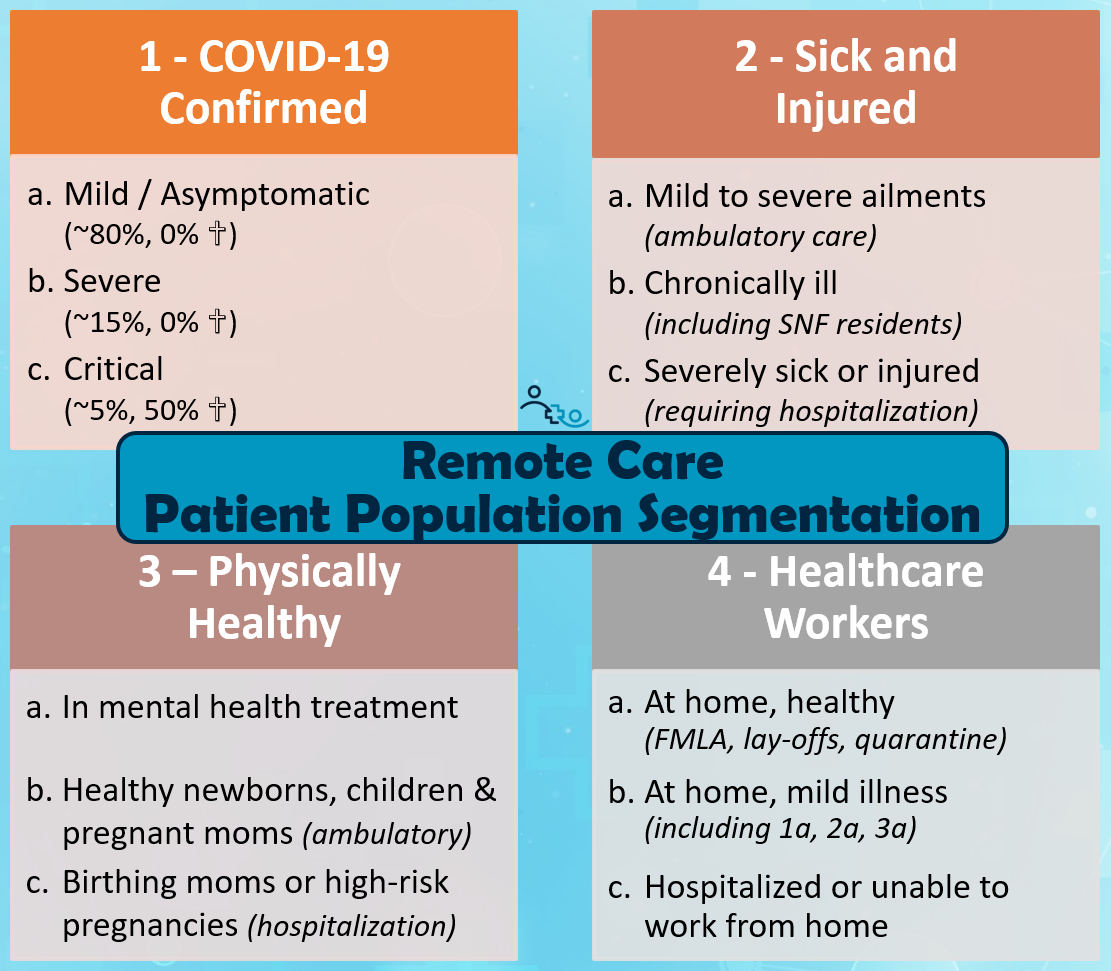


3) The Physiologically Healthy
3a) Requiring mental health treatment (outpatient)
3b) Newborns, toddler, children & pregnant moms (ambulatory)
3c) Birthing moms or high-risk pregnancies (hospitalization)
4) Healthcare Workers
4a) At home, healthy, due to FMLA, lay-offs or covid-19 quarantine
4b) At home, Sick with mild symptoms (including 1a, 2a, and 3a)
4c) Unable to work from home
Telemedicine
Given the non-negotiable need for absolute physical distancing, no patient should be required to venture into the community to visit a medical facility unless absolutely clinically necessary. Given the advancements in technology over the last 10 years, we now have a host of proven, reliable, secure, user-friendly solutions that can provide appropriate and safe clinical care at a distance.
I am, of course, talking about telemedicine.
Each of the 12 population segments listed above (and especially those in categories 1c and 2c) will greatly benefit from the judicious and proper implementation of clinically-designed telemedicine services. Whether you are a concierge physician, an urgent care clinic, a group clinic, a rural FQHC, an urban community health center, or a small health system or critical access hospital. We all must work together to make the feasible technology of telehealth a reality for all Americans. So that all of us can have safe, rapid access to clinically sound care. The goal is to keep as many people as possible out of the hospital so we can protect and save those that become critically ill from Covid-19.
Telemedicine Solutions Menu
Here is a brief menu of just a few high-level telehealth solutions and how they can be used to serve those populations:
1. direct-to-home live audio/video telemedicine (“interactive patient care”, IPC) for 1a, 2a, 3a, 3b and 4b; with healthcare workers under 4a being able to provide clinical care while being home-bound
- keeping these patients out of our health system facilities improves capacity, reduces the use of personal protective equipment (PPE) and contributes to physical distancing
2. remote physiological monitoring (*RPM”), coupled with interactive patient care primarily for 2b and some of 1b and some high-risk pregnancies under 3c
- keeping those vulnerable patients away from potential exposure
- preventing the decompensation to the state of requiring emergency care or hospitalization through vigorous monitoring and detection of early onset
- keeping home health workers mostly distanced, allowing them to focus on the cases that indeed cannot be treated solely remotely
3. TeleICU and remote critical care using stationary IPC and RPM equipment in the ICU and mobile equipment (manual and robotic carts) on the hospital floor for populations 1b, 1c, 2c and 3c
4. interactive patient care with exam capabilities
- those could also be deployed alongside the same populations as for RPM; potentially in a mobile fashion handled by trained “telepresenters”
5. self-service solutions through patient portals, including teleeducation on
- patients need access to clinical information to coordinate their care and given the remote work environment few healthcare organizations can aid in the creation of paper documents
Guidance for Healthcare Leaders
Most health systems we’ve heard about are focusing on building capacity for the anticipated surge in severe to critical Covid-19 cases at a rate of 15-20% of confirmed cases in addition to the base critical care case load.
What health systems may not be focused on yet is to offer alternative solutions to their ambulatory care offerings and to prevent the exacerbation of the chronically ill’s health. As one anecdotal example illustrates, one 80+ year old neighbor of one of us had 3 pre-scheduled appointments canceled with no offering of an alternative, such as direct-to-home telemedicine, which may lead to an undetected and untreated decompensation, potentially resulting in a hospitalization that could have been preventable.
Yet even those that are implementing telehealth are rarely doing it in a thoughtful, orderly pace. Those new to telehealth focus too much on the technology and step over the complexities of clinical workflow design, well-defined and enforced policies, proper training and a mindset of continuous refinement and improvement.
And then there are those who are not doing anything at all, holding on to their long-held belief that telehealth is not for them or their patients and hiding behind red herrings such as not feeling comfortable without being hands-on or the onerous task of obtaining consent in a physical distancing world.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment