The efficacious use of telehealth, as I emphasize often, is first and foremost an exercise in well executed change management. The ADKAR® model (developed and promoted by Prosci, Inc.) postulates that change is only successful and lasting when Awareness, Desire, Knowledge, Ability, and Reinforcement are attended to.
In organizations, the basic form of training (“education”) provides Knowledge and raises Awareness, whereas instructional training provides the learner with the Ability and often also with the Desire.
The right combination of education and (instructional) training thus forms the basis for a successfully optimizing telehealth, so clinicians are empowered to wield this clinical tool to deliver care at a distance most effectively.
Who needs to know?
Telehealth, as a way to deliver care “at a distance”, requires the engagement and contributions of the whole healthcare team to support the variety of telehealth workflows, including scheduling, rooming, billing, etc.
Thus training involves virtually (no pun intended) everyone at the organization — schedulers, medical assistants, nurses, advanced practice providers, physicians, counselors, patient service representatives, coders, IT, compliance, public relations, as well as operational and executive leaders.
Nearly everyone plays a small or big part in creating the telehealth experience and, therefore, should be trained.
What is there to know?
Imagine that you are a new clinician or a new staff member that joins your organization. What would they have to know in order to be “full trained” in telehealth? Turns out there are actually quite a few aspects that enable excellent telehealth:
- Telehealth Policy: the rules and laws that must be adhered to achieve compliance.
- Telehealth Workflows: the various processes involved in scheduling, delivering, and billing telehealth services.
- Telehealth Technology: the technology to conduct telehealth (e.g., solutions for video visits, virtual exams, or remote physiological monitoring) and also the technology for scheduling telehealth visits and documenting telehealth-specific information.
- Telehealth Support: operational, technical, and sometimes optimization and launch support.
- Webside Manners & Virtual Exams: tips and techniques for the effective and proper behavior for video visits and video exams.
- Clinical Guidelines: internally developed, pragmatic guidance on the appropriate use of telehealth as a care delivery modality.
- Telehealth Strategy: a description of the organization’s vision, objectives, roadmap and other elements.
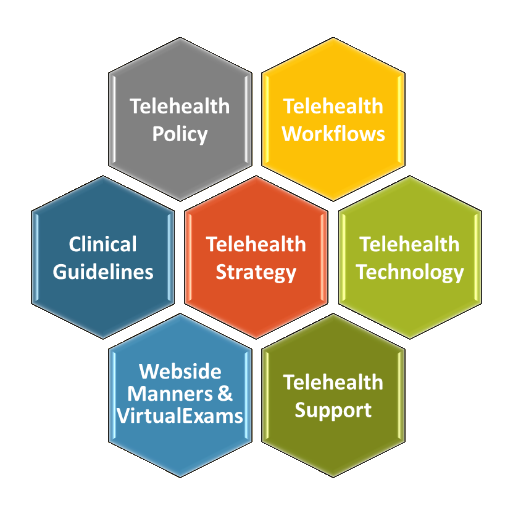


The 7 Levels of Telehealth Training
All these elements together form the foundation for a successful telehealth program. Once they are fully developed, the appropriate staff must be trained on each of the relevant elements.
E.g., while clinicians probably need education and training on all of these elements, front office staff may only require education on the telehealth strategy (“why are we doing this?”) and on the telehealth workflows pertinent to their involvement in telehealth scheduling or providing telehealth support to patients.
Here are the 7 Levels of Telehealth Education and Training:
- Telehealth Policy Education: A review of what is expected, what is permitted, and what is not allowed.
- Telehealth Workflow Training: Reviews and walkthroughs with the respective workflow actors and users on the various process steps that involve each role.
- Telehealth Technology Training: Demonstration and hands on experience in the use of telehealth technology for everyone involved, including clinicians, MAs or nurses, schedulers, and IT support staff.
- Telehealth Support Education: Oftentimes embedded in the workflow and technology training, this training provides information about how and where to get help for any problem that arises.
- “Webside Manners” and “Virtual Exam” Training: A live demonstration and discussion of the best practices on how to conduct virtual visits and virtual exams, ideally with a hands-on practice labs in an all-clinician environment.
- Clinical Guidelines Training: A guided review and discussion among clinicians of each speciality (e.g., primary care, behavioral health) as to the appropriate application of the various virtual care modalities.
- Awareness Training: Raising the awareness (and ideally creating the desire) among clinicians and staff, often in the form of the executive leadership team’s sharing of the vision for telehealth and digital health.
An 8th level of training is just-in-time Telehealth Technology Training for Patients. In the case of video visits, a quick 10 minute Telehealth TechCheck a few days before the visit can give patients who are using telehealth for the first time a brief overview and orientation.
By the way, if lack of provider buy-in is one of your biggest challenges, I encourage you to invest in training to cover “webside manners” and “virtual exams” (#4). The lack of any information is the primary root cause for the reluctance by many clinicians to use telehealth. But that’s a topic for another week.
Which of these trainings are you delivering to your staff and providers at your organization? Which ones are you missing?








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.








