Wicked problems are challenges that are tricky or impossible to solve due to the intertwined nature of the various factors and root causes that create the problem, most of them being difficult to even identify or correlate.
Wicked Problems, by definition, cannot be solved by a single solution or even a set of solutions. At best, the effects of Wicked Problems can often only be partially alleviated.
Here are just a few of the characteristics of Wicked Problems, taken from the 1973 paper by Rittel and Webber:
- There is no definite formulation of a wicked problem.
- Every wicked problem can be considered a symptom of another problem.
- Solutions to wicked problems are not true-or-false, but better-or-worse.
- There is no immediate solution and no ultimate test of a solution to a wicked problem.
- Every wicked problem is essentially unique.
The shortage of nursing staff is one example of the effect of the underlying wicked problem which spans multiple root causes — the great resignation, effects of the Covid-19 health crisis, systemic overwork, inefficient systems, user-unfriendly technology, overuse of traveling nurses, outdated physician-nursing hierarchy, shortcomings in nursing education, just to name a few.
Telehealth to the Rescue!
While telehealth cannot solve the wicked problem, it can alleviate the effects of the nursing shortage and chip away at some of its causes, such as stress, burnout, lack of coverage, etc.
Here are several ways how Telehealth can serve as a solution — or rather a set of solutions — to alleviate the nursing shortage.
Telehealth Workflow Design: Much of the stress in nursing is caused by poorly defined processes, especially the hand-off points from and to other workflows. By focusing on the design of proper telehealth workflows, many stressors can be removed for nurses (and clinicians, too). While, ultimately, all processes should be optimized, it is much easier to start to train on a new process vs. trying to change the established habits.
Telehealth from Home: Much of the demand on nursing in ambulatory care originates from the need to support multiple providers, oftentimes to cover for the existing shortage of nursing resources. By allowing providers to conduct telehealth visits from home a few times a week, many of the nursing tasks typical for in-person care can safely be omitted. While “TeleRooming” as well as “TeleFollowUp” for some patients is still needed, not all patients may require a nurse to be involved in these steps, thus freeing them up for other tasks.
Telehealth Support from Home: A change of pace and scenery can do wonders to alleviate stress and burnout. To support an ambulatory practice, nurses can support telehealth visits from home, including triage, rooming, and post visit tasks.
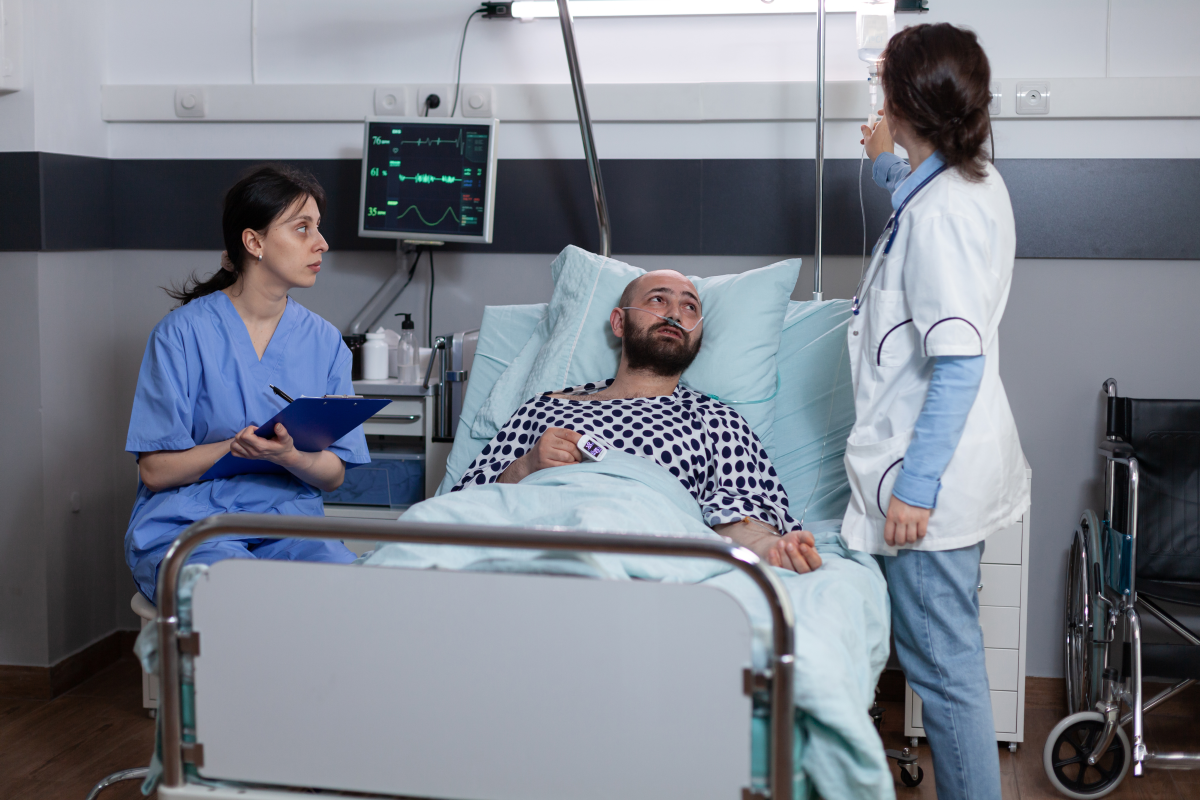


Virtual Nursing. But even in an in-patient environment, virtual nursing can be viably integrated into the bedside workflows to offload suitable nursing tasks. Tasks such as discharge planning, medication reconciliation, completing procedure checklists, answering questions, etc. can all be conducted remotely.
Remote Physiological Monitoring (RPM). In the critical care environment, the reliable integration of remote physiological monitoring has been demonstrated for two decades in the form of Tele ICUs. Similarly, RPM solutions can also be deployed in non-critical environments in hospitals or skilled nursing facilities. A single central monitoring nurse that also has bidirectional video chat access to the patient, can safely monitor and care for a multitude of patients. This relieves the “on-floor” nurse from false alarms or simple requests.
Nurses – A Heroic Army in the Healthcare Forces
My introduction to the amazing contributions of nurses came almost 20 years ago at the Mayo Clinic. After having been trained in contextual inquiry and armed with a notebook and a digital camera, I shadowed nurses on an inpatient unit. What an eye opening, transformative experience!
While our focus was on improving medication administration (another wicked problem), the amazing insight I gained was just how complex a seemingly relatively simple task as hospital nursing is! The patient care part, aside from a few patients with taxing personalities, was almost the easy part.
What was much harder to master was the sheer number of interruptions at virtually any given time: Communication with unit secretaries, custodial staff, lab technicians, other nurses, physicians, residents, administrators, families, and, of course, patients. Mastery of multiple skills such as administering drugs, charting, changing, assisting, teaching, transferring, coordinating, double-checking, and communicating.
Everybody in healthcare plays an important role to make extraordinary care possible. But from my vantage point, nurses are the glue — the connective tissue, if you will — that holds it all together.
So let’s explore the use of telehealth to alleviate the problems caused by the nursing shortage and even start to overcome some of those obstacles.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.








