Don’t Blame the Users…



Here are the 5 most important results that every telemedicine service should achieve:
- High Physician Satisfaction
- High Patient Satisfaction
- Financial Sustainability
- Positive Clinical Outcomes
- Strategic Relevance
At the top of the list of results that telehealth must achieve is high physician satisfaction. Unlike many other strategic goal setting efforts, achieving physician satisfaction is not mutually exclusive with any other goals. Rather it is a force multiplier in helping to achieve the other goals, such as financial sustainability or positive clinical outcomes.
When applying the principle that every system is perfectly designed to get the results it gets, we shift any blame for unwanted results from the users of the system to the system itself. So in order to get the results we want, say, a high degree of physician satisfaction, we need to study the system that creates or influences the satisfaction (or dissatisfaction).
…blame the system
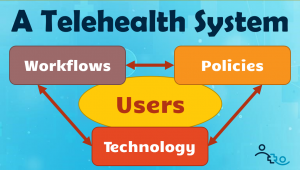


Here are examples of the various elements of these three categories:
Workflows
- scheduling appointment
- TeleRooming
- conducting virtual visit
- post-visit activities, e.g., prescriptions, follow-up visits, labs, radiological exams
- billing processes
- etc.
Policies
- “webside” etiquette
- patient safety
- informed consent
- physician licensure
- clinical guidelines
- etc.
Technology
- secure video chat app
- electronic medical record
- patient appointment system
- clinician hardware & connectivity
- patient hardware & connectivity
- ePrescribing solution
- etc.
As you can see from this incomplete list, telehealth is a system with many different elements, many different users and many different objectives that all must be aligned to work together. Which is why it takes a village to make telehealth truly a success.
Creating Telehealth Success
The bottom three of the top five concerns (financial sustainability, positive clinical outcomes, and strategic relevance) are relatively easy to address.
Financial Sustainability comes from the rigorous checking that the services being scheduled and delivered are (still) reimbursable. Financial Sustainability is also achieved by shifting providers away from lower-reimbursed telephonic visits to higher-value E&M visits using live audio/video. To achieve Financial Sustainability, the systems’ workflows and policies must implement this priority on reimbursability.
Positive Clinical Outcomes can be influenced by making it easier for patients to get timely access to care (which virtual care without the overhead of traveling can conveniently accomplish), by offering ad hoc virtual care and by employing more advanced telehealth services such as remote patient monitoring for chronic care management or readmission prevention. This result is an intrinsic outcome of a telehealth service well designed, but only if the service is marketed properly to those patients, for whom telehealth can make a positive difference.
Strategic Relevance comes from consciously and carefully choosing the right telemedicine services that will advance the organization’s overall strategic objectives. Just like positive clinical outcomes, it is a welcome “by-product” of a well implemented telehealth service.
Achieving Satisfaction
Let’s be clear once more. Telehealth is a service, delivered by people to other people. It is not a technology, but rather a clinical tool clinicians can consciously employ to give patients access to care when they need it where they want it.
For patient satisfaction to be created, focusing on physician satisfaction first is critical. Without a confident, satisfied “video presence”, patients will not feel comfortable with the visit and will not really like it, no matter how convenient.
Looking at the challenge from a systems perspective, to achieve high physician satisfaction, we must focus on getting all the workflows and all the policies lined up to support the clinicians in their job to apply their clinical expertise to the patient’s condition, with as few distractions as possible.
Thus the first focus lies in the conscious and careful design of the workflows, optimizing the experience for all involved (not just the clinicians) but also the patient (e.g., by doing a pre-visit TechCheck) the billing team (by giving them a heads up of a newly scheduled visit, so they can verify the eligibility), the schedulers, the nurses, the MAs, etc.
Next, policies need to be carefully designed to adhere to the laws, the regulations and best practices (e.g., clinical guidelines). As much as possible, all stakeholders (i.e., those affected by the policy) should be involved in the iterations of the policy to provide feedback or input or at least just stay in the loop to understand the policies evolution.
Finally, whatever technology you go with, make it a conscious choice to select a technology that supports your desired experience for the users of each technology. And if there are some idiosyncrasies, by involving the staff and the clinicians in the process of selecting and configuring the various technologies, you build the buy in. Of course, even for the most tech-savvy person, it’s always a best practice to develop a quick cheat sheet or a video tutorial or have someone give a brief 1:1 demo to ease any trepidation about how to best use the technology.
Getting the Results You Want
The secret, and the hard work, of making telehealth successful lies in understanding that telehealth is a system of workflows, policies and technologies and that each element should be consciously selected or developed, using as much input from all affected stakeholders as possible. It’s a small “price” to pay for a big pay off when everyone has strong ownership in “their telehealth service”.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment