One of the aspects of telemedicine (“practicing medicine at a distance”) is that it is not just another healthcare IT project.
In healthcare IT projects, typically a need is identified (a new image management system, new business intelligence software, or even a new EMR) and the IT team peruses its vendor network, attends conferences and scours the web to find the one vendor whose solution will (a) fit the IT department’s technical paradigm, (b) interface with or at least play well with the existing technologies, and (c) kind of do what the users want it to do.
A large portion of the IT team’s and the organization’s effort and time (sometimes upward of 40%) is expended on finding the right vendor with the best solution and negotiating the most favorable deal. Another large portion of effort is then spent on installing, configuring and training the users on the selected solution and “getting it to work” in the organization’s organically grown maze of clinical and administrative applications.
Another distinction is that most healthcare IT solutions are either used by a small number of people (or a specialty, such as radiology or oncology) or by everyone in the organization (like an EMR or a human resources management system).
Telemedicine, by definition (“practicing medicine at a distance”), is different. In Telemedicine it is not first and foremost about the technology. It is about delivering care and practicing medicine – the core raison d’être of the organization.
Launching a telehealth service is about launching a new clinical service offering. Yes, it (mostly) uses the same physicians, the same staff, the same buildings and the same specialties. But it is a completely new service, that requires a different approach than simply selecting and installing a new piece of software.
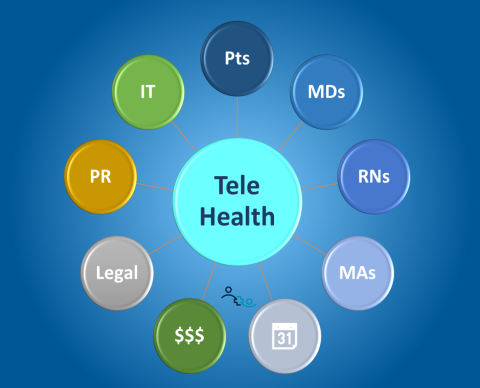


Telehealth is Healthcare
A Telehealth service not only involves patients and physicians, it also affects the nurses, medical assistants, schedulers, billing, legal, public relations, and (of course) the IT department.
Telehealth visits, just like any other healthcare visit, need to be scheduled, prepared, conducted, and billed. They need to be promoted and adhere to all the legal rules and regulations.
In that sense, telehealth is truly the same as traditional in-person healthcare delivery. I guess the only things telehealth does not need are wayfinding, valet parking and a patient cafeteria.
By virtue of the patient and provider being physically separated, complexities arise from keeping the workflows on both sides in sync, which is tricky since many healthcare services do not run like a car manufacturing floor. Physicians run behind due to a patient needing special attention and patients may encounter technical problems or delays of their own.
Thus, while telehealth is healthcare, it is actually, in some regards, a more complex form of care delivery; at least with challenges we have not had to deal with before.
Case Study: A rural FQHC village
I recently worked with a rural FQHC that had just launched a school-based telehealth service providing the students access to the pediatric offices 30 minutes away from the school. In the process of standardizing their service, we identified the need to define a number of workflows such as
- schedule an ad hoc same-day appointment (e.g., determining eligibility, obtaining consent for telemedicine)
- establishing a new patient (i.e., if the patient had not been seen before)
- prepare for the visit with the provider (e.g., taking images and vitals before the visit)
- conduct the telehealth visit (e.g., sending prescriptions and communication of care plans to the parents)
- post-visit activities (e.g, completing clinical documentation on both ends, following up with parents)
Another side effect of telehealth was that initially the workflow and technology selection now required manual documentation in three different electronic medical record systems (the school’s, the pediatrician’s and the telemedicine solution’s EMR).
In the process of streamlining and optimizing the service, I enlisted the support of the following people:
- the billing manager (to determine eligible payors)
- the schedulers (to make sure the visit is set up as a telehealth visit)
- the legal counsel (regarding the consent form)
- the medical assistants in the pediatrics office (to prepare the patient record for the provider based on the school nurses’ information)
- the quality officer (to obtain reports on the performance of the services)
- the technical lead (to set up a process for technical support)
- the EMR specialist (to configure the EMR for telemedicine)
- the public relations manager (for an internal newsletter and also for their quarterly patient-facing publication)
- the Associate Medical Directors (to inform them of the progress and availability of telemedicine in their practices)
- the COO (to ensure technical and operational support)
- the CFO (to ensure his okay on writing off non-billable services)
- and the CEO (to ensure strategic support for the service to remove any possible barriers)
Every one of these people in this “FQHC village” made their contribution to ensuring that the service can run smoothly and that the students, the parents, the school nurses, the providers, the medical staff, the billing staff and the schedulers are all having a satisfying experience for each telemedicine visit.
And that’s what I mean when I say that “Launching Telehealth is about launching a new Clinical Service”, “Telehealth is Healthcare” and that “It takes a village to raise up a new telehealth service.”








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment