Over the last few weeks, Telehealth Tuesday has covered the various facets of Telebehavioral Health and how to take your Telebehavioral Health service to the next level. In this week’s column we’re applying the concept of measuring telehealth success to Telebehavioral Health, a key step toward improving the performance of your Telebehavioral Health services.
Key Performance Indicators (KPIs)
Key Performance Indicators, or KPIs, are a frequently used business tool to help leaders to keep a close eye on the performance of an organization, a team, or an individual service, such as Telebehavioral Health.
With renewed focus on the financial performance of healthcare, it’s a good idea for healthcare leaders at all levels to take note of the principles that have successfully been used in other industries, KPIs being one of them.
The goal is to find the vital few metrics that can accurately answer the critical questions that leaders are asking: the key indicators of the telehealth service’s performance.
For a Telebehavioral Health service, there are many things you can measure: minutes spent online, the ratio of video to phone calls, the miles patients saved by not having to drive to the clinic, revenue generated, the number of averted hospitalizations, and maybe even marriages saved.
But not every measurement is a good indicator of the service’s performance and it is critical to identify the key performance indicators (KPIs) that provide the leaders with actionable data.
Telebehavioral Health Performance Objectives
In the last article I introduced six objectives that are critical for most Telebehavioral Health services, especially those launched in 2020 in response to the Covid-19 health crisis.
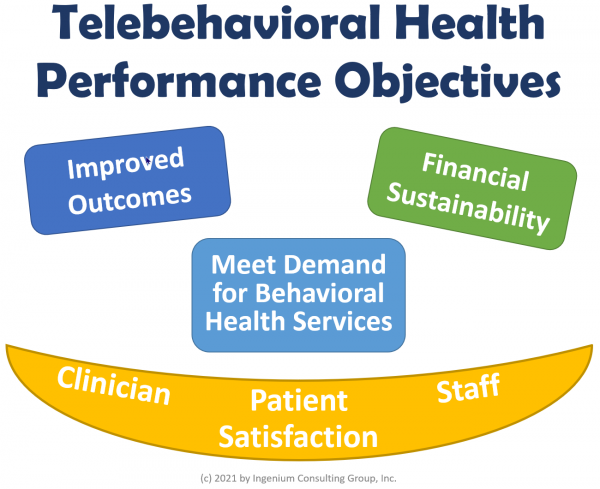


In that article I discussed the first two, Improved Outcomes and Financial Sustainability. Let me describe the remaining objectives before we come back to the topic of KPIs.
3. Clinician Satisfaction
High clinician satisfaction is a key performance objective, because without the clinicians support and engagement, no Telebehavioral Health service will ever be high performing. Many organizations in other industries put the needs of the customer first, but it is the really great organizations that treat their staff and employees right.
I am truly convinced that of all the objectives for any telehealth service, clinician satisfaction is the most important one. Which is why I highly recommend that organizations adopt a “Physicians’ Bill of Telehealth Rights” to publicly declare their commitment to creating a satisfying experience for clinicians.
Clinician Satisfaction can also have a high impact on Financial Sustainability. In the current competitive environment, clinicians may be seeking other employment opportunities if they are not satisfied and patients, who have an increasing menu of online offerings, may also “quit” their counsellor if that counsellor does not seem too happy with the provision of Telebehavioral Health.
4. Patient Satisfaction
Patient satisfaction is closely related to clinician satisfaction: without an engaged clinician that is confident in the use of this new technology, very few patients will have a stellar experience or would recommend the experience to “friends and family”.
Patient satisfaction is also the underlying first step toward achieving improved health outcomes. This is more important in Telebehavioral Health than in any other clinical specialty. Without the engagement of the patient in their care plan, in their treatment, the achievement of outcomes is elusive.
5. Staff Satisfaction
Finishing out the trifecta of satisfaction (illustrated as a smile in the graphic) is the satisfaction of the staff. While not as critical as the clinicians’ satisfaction, the staff’s satisfaction (or rather their dissatisfaction) will have a great impact on the physician’s satisfaction and, in the case of scheduling appointments or collecting co-pays, also on the patient satisfaction.
6. Meet the Demand for Behavioral Health Services
This performance objective may be the odd one out, but it is one that is on most behavioral health services leaders’ minds. For years, if not decades, we have experienced a shortage of qualified behavioral health providers and access to behavioral health, even before the Covid-19 health crisis, has been inadequate at best.
Therefore, this objective does not only aim at the performance of the behavioral health team, but at its responsibility to the greater good: “how can the limited resources we have be optimized so that we can serve as many clients as possible?”
Key Performance Indicators for Telebehavioral Health
The purpose of KPIs is to select the few metrics that give the best indication of the aspects of performance that matters.
I propose that the six performance objectives laid out above (health outcome, financial sustainability, satisfaction and meeting the demand) are in alignment with any healthcare organization’s strategic objectives of growth, finances, health, people, and community.
So what are the Key Performance Indicators that can give a good indication of how well your Telehealth Service is performing? Specifically for Telebehavioral Health, here are five key metrics to get you started:
1. No Shows: measuring no shows as a ratio of appointments; also track the number of appointment slots unfilled. Lower no shows for a particular patient can improve outcomes, improve financial sustainability, create a higher satisfaction for clinicians and staff (no shows are frustrating and create more work) and for the patient. Finally, fewer no shows and no unfilled appointment slots lead to increased productivity and the team can serve more patients.
2. Periodic Clinician, Staff Satisfaction: Occasional collection of satisfaction data for a day on all patients will provide insight, gives the team a chance to share ideas for improvements, and in general sends the message that their opinions matter. When properly designed and analyzed, measuring satisfaction can also lead to improved support and training that further improves satisfaction.
3. Client Net Promoter Score (NPS): Assessing how likely a client would be to recommend Telebehavioral Health with this counsellor or psychiatrist to a friend or family member. World-class service companies like Disney range from +50 to +70 (on a scale from -100 to +100) and I have repeatedly seen NPS for Telebehavioral Health services in the +70s.
4. Telehealth Visits by Modality: full reimbursement for telephonic care, while currently paid for and preferred by many clinicians and, by extension, their clients, is no longer a viable strategy. Forward looking leaders use this KPI to calculate their financial exposure should reimbursement for audio-only drop to a fraction or to $0 altogether.
5. Technical Performance: Even though Telehealth is not about the technology, if the technology is cumbersome to use, unreliable, or inaccessible to your clients due to coverage or bandwidth limitations, then finding out what your clients, your clinicians, and your staff are thinking about the technology is crucial to bringing the satisfaction scores up and with it improving the outcomes and the financial sustainability.
A final word on Measuring Success
Collecting and analyzing metrics can be quite expensive, so leaders want to make sure they are only collecting those metrics that they can also act on to make a difference. The five KPIs we identified above may not be the ones your organization needs. But it is imperative that you identify the ones that apply to your organization.
If you’d like to discuss how you can set up a telehealth performance management system at your organization, contact me through any of the options below.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment