Over the past two years I have talked about telehealth with leaders at over 30 community health centers, rural health clinics, behavioral health clinics, and health systems. Based on our conversation, most of them are pretty much in the dark when it comes to the performance of telehealth at their organization.
While many assume or are even aware that telehealth is being conducted by the clinicians of their organizations, not a single one had an actual handle on how many telehealth visits were being conducted in recent months — and how many of those visits actually involved video (vs. audio-only).
Not knowing how telehealth is doing can be a critical problem in the context of an increasing expectation by the Modern Healthcare Consumer to receive telehealth when they want it and when it’s clinically appropriate coupled with an increasing competition by regional healthcare providers (especially larger health systems, as outlined in this May 2022 HBR article) and payers (such as United Health moving toward a “virtual first” model for its health plan members).
There are two major critical challenges resulting from not knowing the performance of your telehealth services:
(1) If your clinicians have by and large reverted back to in-person care based on their personal preference (given a less than stellar experience doing telehealth in the early days of Covid), you may be losing patients that have sought telehealth but were not able to get it.
(2) If your clinicians are providing telehealth, but receive little support, the experience may be frustrating and subpar for both clinicians and patients alike. With proper workflows, proper training, proper support and proper technology, virtually all telehealth visits can create a high quality, satisfying care experience.
Not doing Telehealth is No Longer an Option
As I’ve started to outline above, there are numerous drivers that are pushing all of healthcare to offer virtual care options. Here’s a quick short list:
Regional Competition: Many academic medical centers and larger health systems had experience with specialty care telehealth prior to the pandemic and which offered them a great head start into telehealth in their behavioral health and primary care services. E.g., within just a few months, Mayo Clinic went from 300 providers to 6,500 providers doing telehealth. These players also have the resources to continuously optimize their telehealth offerings and with the lack of geographic limitations, are expanding their service areas.
Self-Insured Competition: As healthcare costs for employers have risen exponentially for decades, many self-insured companies are seeing great opportunities to lower the cost of care by leveraging telehealth to address the problem. Examples include Walmart Health and Amazon Care who are moving toward a “virtual first” model, alongside with payers such as United Health (see the article referenced above). In these models, employees’ health is taken care of internally first, before “handing them off” to other healthcare providers.
Virtual-Only Competition: Whether it’s cash-pay telehealth services that offer a quick, smooth care experience by being designed around the patient experience, or whether it’s virtual-only service firms (such as Teladoc, AmWell, MD Live, etc.) that have been contracted by payors to offer a “first level of care” — patients have increasingly alternative options to receive care virtually, if they so chose.
The Modern Healthcare Consumer’s Willingness: According to numerous surveys, the majority of patients that received telehealth, would do so again within the next 12 months. Even in the baby boomer bracket.
The Modern Healthcare Consumer’s Needs: In our increasingly busy world, especially those with limited access to care can often not afford transportation or don’t have the time to fit a 1-2 hour visit into their schedule. Telehealth offers a convenient alternative that leads to fewer no shows, fewer cancellations and a higher continuity of care.
Increasing Evidence of Equivalent Efficacy: As the use of telehealth continues, numerous studies are indicating that telehealth, under many circumstances, can be just as effective as in-person care — if the workflows and technology are properly designed, of course. And a video visit is always much better than no visit (or even a phone call) anytime.
The Side Effects of Bad Telehealth
I’ve already alluded to it in some of the comments above, but wanted to explicitly point out what may be hiding below the tip of the telehealth iceberg that a leader may only be seeing. Here are some of the most common and egregious side effects that ultimately will make it so much harder to integrate telehealth into a hybrid care model:
1. Poor Patient Experience and Patient Attrition — while patient satisfaction with telehealth is typically very high, it is largely because patients are mostly grateful for the convenience that receiving care at home presents. But direct-to-consumer telehealth with bring-your-own-device technology is one of the top 5 most challenging flavors of telehealth.
Patients now find themselves in a fiercely-competitive landscape that knows no geographic boundaries. Once they have experienced a smooth, professional, awesome telehealth visit vs. one fraught with technical glitches, confusing communication and not-very-confident and not-very-professional-looking physicians (e.g., grainy picture, poor lighting, awkward face framing, distracting background, etc.) — patients, when given the choice, very clearly know which telehealth provider they will want to use in the future. They will take their virtual care needs elsewhere.
2. Poor Financial Performance and Legal Risks — the reimbursement landscape for telehealth shifted dramatically in March 2020 as widespread social distancing took hold and Medicare, Medicaid and commercial payors opened the telehealth floodgates to ensure that care could be delivered to those who needed it, without the fear of diminishing revenue. But the playing field is not the same across all clinical specialties, provider levels, and definitely not across all payors. As we are approaching the end of the Public Health Emergency (PHE), it takes a tremendous amount of attention to detail to stay abreast of the rapidly changing reimbursement landscape.
Traditionally, the billing team is at the tail end of a healthcare organization’s money trail and other than the occasional reject claim, the tail would never “wag the dog”. But telehealth requires a very different mindset. If not implemented well, telehealth can hurt the financial performance of an organization by rendering non-billable services or by leaving money on the table by not taking advantage of the new ways to provide remote care that is reimbursable.



3. Frustrated Physicians — while physician buy-in into telehealth has historically been low, virtually all physicians that I have worked with over the past 10 years have come to like and even love telemedicine as an effective way to deliver care to their patients. Among my colleagues I’m known as the “physician whisperer” for my ability to turn vigorously-opposed clinicians into telehealth zealots (though I can’t do much for resigned, apathetic providers).
The majority of physicians understood the need for telehealth during the beginning of the health crisis and were professionally willing to plow through the discomfort and challenges, because their patients need this service. But as soon as we could go back to in-person care, clinicians were the first to advocate for patients coming in to see them in person.
While the opportunity for a great first impression has been lost, now is the time to re-engage with clinicians and design a telehealth experience around the needs of the clinicians and the patients.
4. Leadership, Staff, and Clinician burnout — And it’s not just the clinicians who are experiencing frustration and burnout with telehealth. It’s front line leaders, schedulers, billing staff, nurses, MAs, etc. who are doing the heavy lifting of making things work. Without adequate support and training, telehealth will continue to be the ugly stepchild of medicine that it became at many organizations in the wake of Covid.


The Cure is Telehealth Optimization
3. The Cure is Telehealth Optimization
Fortunately, fixing the problems is not quite rocket science, though it’s also not as easy as putting on a band aid. Some surgery (in the form of organizational change) is needed to make sure that your organization and your patients are getting the most value out of telehealth.
What it takes first, is leadership: a commitment to develop a telehealth strategy, establish a telehealth governance team, and identify qualified operational and technical support staff. Next, it’s about optimizing the telehealth workflows, creating appropriate policies and making sure that the selected technology is adequate to satisfy the needs of clinicians and patients (and not just the needs of IT).
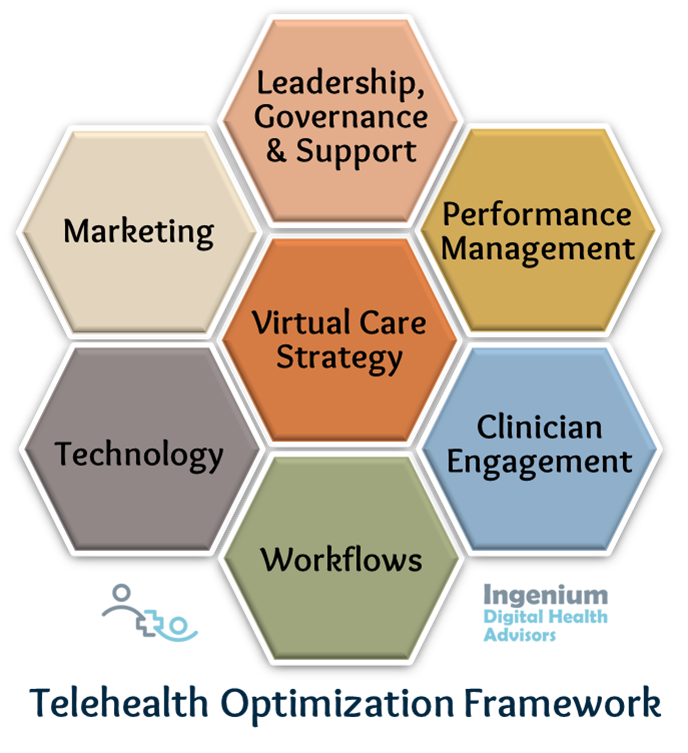
In short, you need to follow a framework for telehealth optimization.
Because that is what should lie beneath the surface of the Telehealth Iceberg: a dedication to deliver extraordinary care, regardless of the modality.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment