Federally Qualified Health Centers hold a special status in the US healthcare system. As part of the healthcare “safety net”, FQHCs offer healthcare to anyone seeking care, regardless of their ability to pay. In return they enjoy a more lucrative standard rate for medical visits to offset the cost of care to those who cannot pay or can only pay very little.
Prior to the Covid-19 health crisis FQHCs were explicitly prohibited to offer telehealth as we now know it to their patients. While they were permitted to facilitate virtual patient visits with far away specialists (oftentimes at academic medical centers), clinicians at FQHCs were not allowed to see patients “in the comfort of their home” — a service that actually is most welcomed by the population FQHCs serve, given the challenge of transportation or even finding the time between low-paying jobs and child care.
Yet Covid changed all of that. While telehealth was previously forbidden (presumably because telehealth “back then” was not considered appropriate for primary care or behavioral health and only was deemed appropriate to offset “long travel distances”) suddenly telehealth was available and quickly taken advantage of.
While many health center leaders are concerned about the telehealth rules going back to pre-Covid law when the PHE and the 151-day telehealth extension ends, others are investing in the likely future of a world where many of the health center’s services can be accessed “at a distance” via telehealth.
A Glimpse of the Future
The question that was posed to me this week (via an invite to speak at a state primary care conference geared at Community Health Centers) sounded daring upon first glance: “What would a virtual health center look like?
Having worked with FQHCs on telehealth for many years now, this question sounds equally dystopian or like heresy. However, as a creative passionate about the future, the “actual reality” of a virtual health center, actually does not sound too far off and may just be the solution to the growing challenge of access to coordinated, comprehensive, quality care.
So, to make this less scary at first, let’s just forward 30 years…lightning-fast internet is ubiquitously available in even the remotest parts…access to affordable, reliable and secure technology is a given. Clinicians are aided by augmented intelligence (the friendlier form of AI) to not only help make sense of the vast amounts of data available about any given patient, but to also provide convenient access to the ever increasing volume of evidence-based insights to aid in diagnosis and treatment.
In this future world, access to care would almost exclusively be achieved virtually, from the comfort of the patient’s home or wherever they may be. In 30 years’ time, the first contact may not even be with a person, but probably with a pleasant, polite, patient and knowledgeable clinical assistant that expediently can get us to the right expert. This would be followed by a virtual (potentially even immersive, as in “virtual reality”) visit with our knowledge-armed clinician.
Primary Care without Exams
But before we get there, let’s first talk about the elephant in the virtual exam room.
Many clinicians still hold on to the notion that, especially in primary care, an in person visit is far superior to a virtual visit. But the current reality is very different. The vast majority of outpatient visits have already been “hands-off”, “exam-free” for many years (if not decades). Most diagnoses are made through the assessment of symptoms and patient history and the analysis of vital signs and lab and imaging tests paired with the clinicians expertise and experience. While hands-on exams are often used to confirm a diagnosis, they are seldom the sole deciding data point.
My personal eye-opening moment came 10 years ago, when a small-town family medicine doctor with 35 years of experience confided in me: “I don’t know the last time that listening to a patient’s heart and lung sounds has made a difference in my diagnosis or treatment. But we go through the “spiel” because our patients expect it.”
At the 2022 MATRC Summit, one physician – an internist with 15 years of experience in telehealth at the Cleveland Clinic – explained in great detail the various ways in which even physical exams can be conducted effectively during a virtual visit.
And if the virtual assessment is inconclusive? Then we do what we often do in healthcare: we order another test, which in that case may be the need for an in-person exam to confirm or make the diagnosis confidently.
The Road to a Virtual Health Center
As an optimist, I don’t think that the vision I painted is 30 years away. But it’s also not going to happen within the next 30 months. The realistic time frame probably lies between 7 and 12 years.
Of course if the Coronavirus crisis with its ever evolving mutations is continuing to make close physical contact dangerous (or at least “unhealthy”), this timeline could greatly be accelerated, just like the “fast-forward button” of Covid-19 showed us for telehealth.
So what is a healthcare leader to do, who wants to future-proof their organization and ensure good access to affordable, quality healthcare for the patients in their area?
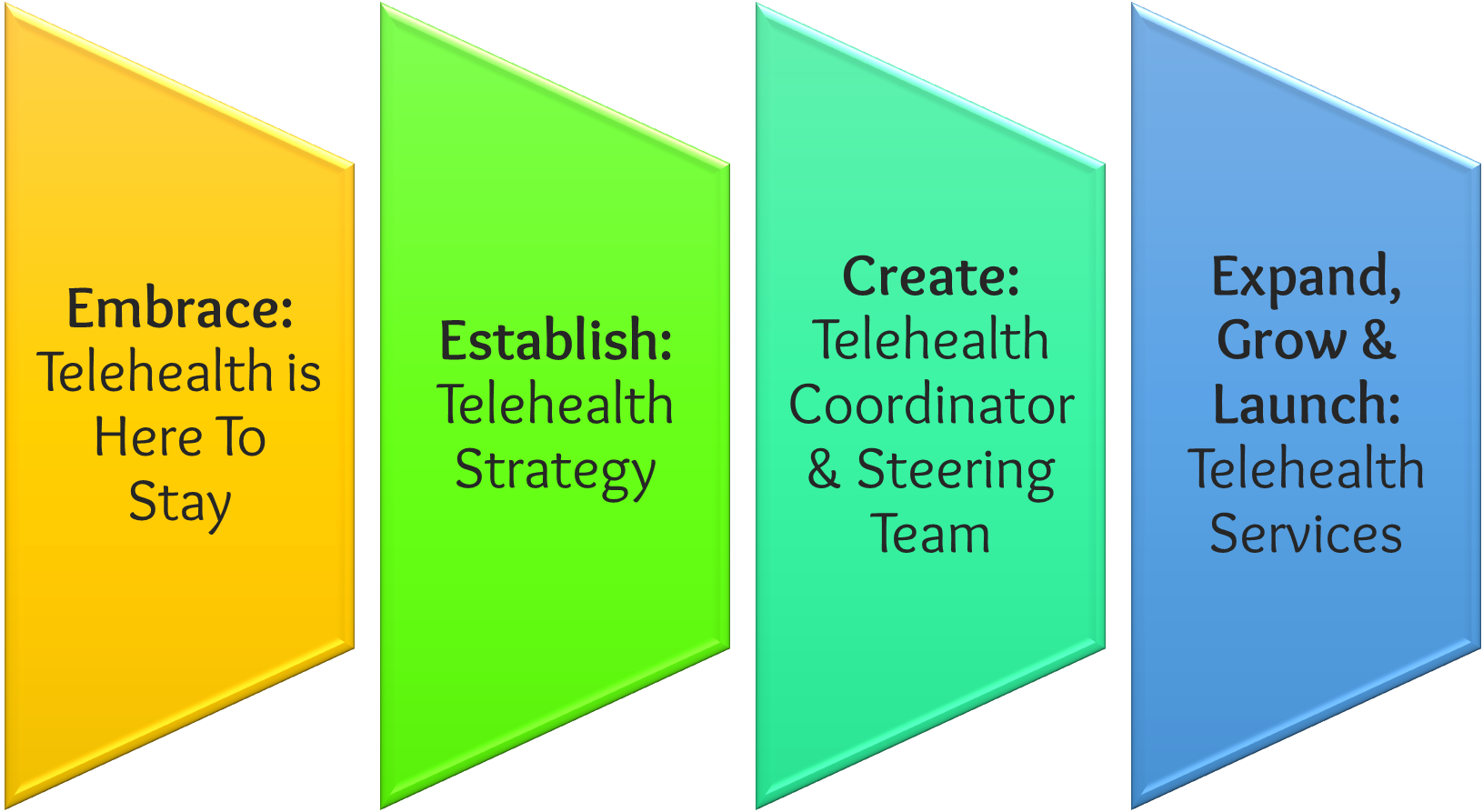


The first action is a mindset shift to not give in to the fears that the system will go back to pre-Covid rules. While, given the political dynamics, the current temporary exceptions may lapse for a few weeks or months, telehealth will not be outlawed again. Especially not for organizations whose mission is to serve the medically underserved.
Even Medicare finally was given by congress what their in-house innovation team had long wished for: a redefinition of the “originating site” now merely stating the obvious of “any site in the United States at which the eligible telehealth individual is located at the time the service is furnished…including the home of an individual.” It took over 20 years to rewrite that statute and now that it has been rewritten, it’ll be quite easy and likely to make it the law.
The original limitations placed on FQHCs and RHCs were in my opinion based on poorly informed knowledge about the possibilities of telehealth — and they were made way back when technology and connectivity were extremely clunky. Yet even before 2019 I worked with FQHCs on “fringe use cases”, such as school-based care, because the leaders believed in the future of telehealth, even in the safety net world.
The second action is the development of a Telehealth Strategy, or even better a Digital Health Strategy. In order to convince clinicians and staff to allow the integration of virtual care services in a hybrid care world, it must be clear to everyone WHY, HOW, and WHEN the health center is going to invest into telehealth.
The third action is to formally optimize your existing telehealth services. Most telehealth workflows and technology are poorly defined as they were thrown together haphazardly at the beginning of the public health emergency. Now is the time to clean up those messy processes and select user-friendly technology, preferably by establishing the role of a telehealth coordinator and a telehealth steering team to perform and manage the optimization.
The fourth action is to first grow and expand your existing telehealth services (e.g., TeleBehavioral Health) and then launch new telehealth services offerings through proof-of-concepts. New offerings can include mobile clinics, digital therapeutics, or remote physiological monitoring services for chronic disease management.
Becoming Virtual
As you progress on these four steps, the gradual shift toward a Virtual Health Center has started. It will take years, if not a decade to substantially shift most of care to a virtual environment. After all, it is also the patients’ choice and connectivity is still quite a problem in many rural areas.
But 100% telehealth (when patients want it, when they can do it, and when it’s clinically appropriate) is achievable — and given the strong virtual competition, it’s a smart if not critical move for any health center leader to future proof their organization and ensure its survival.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment