The Covid-19 health crisis quickly turned everyone’s attention to telehealth as a means to keep providers and staff safe and patients both safe and healthy. Most organizations very quickly stood up telemedicine without the knowledge on how to properly launch this new clinical service offering. Now, in 2021, most organizations are taking a step back to evaluate how to sustainably integrate telehealth into their offerings in the long run.
The Key Characteristics of Mediocre Telehealth
In many organizations telehealth has fallen short of the expectations, with utilization across many outpatient services dropping back in the low single-digit percentages of overall volume in the summer of 2020.
Through our work with many healthcare organizations, we have identified these key three most common characteristics of telehealth services that are underperforming.
- Low Physician Satisfaction and Engagement
- Low Patient Acceptance and Patient Satisfaction
- Poor Financial Performance
Low Physician Satisfaction, if not formally measured, often manifests through a reluctance to fully engage in leveraging telehealth to provide patients with access to care. Explanations range from a lack of acceptance by patients, technical and connectivity challenges on the patient end, or the notion that “telehealth is simply not clinically appropriate” for care.
Low Patient Acceptance and Patient Satisfaction in most organizations goes hand in hand with a low adoption of telehealth by the clinicians. While rarely measured formally, the lore is, anecdotally, that “patients are just not comfortable with telehealth”. While, especially in rural areas or in organizations serving populations with a low socio-economic status, access to technology or the availability of reliable (and affordable) internet connectivity can be a real barrier, the vast majority of patients do enjoy the convenience and (Covid) safety that telehealth affords and will find ways to get connected. Most of the time patient satisfaction with their physician also takes a dramatic hit when the clinician (see above) is reluctant to fully use telehealth, most often feeling not as confident with telehealth as with the in-person care setting.
Poor Financial Performance is the final of the three most common characteristics and I’m referring here to an apples-to-apples comparison, i.e., pre-Covid-19 outpatient service revenue vs. current revenue. While a reduction in visit volumes due to Covid-19 concerns is partly responsible for a drop in volume, many successful organizations have shown to actually increase visit volumes by fully embracing a hybrid care delivery model that provides 50-60% of its care virtually. Another challenge for the financial performance is the reduced reimbursement for audio-only, telephonic telehealth, which can be minimized by increasing the utilization of live audio/video telehealth. While many payors, during the ongoing health crisis, have pledged to pay for telehealth, some are also now planning to reduce the reimbursement rate, even for live audio/video, compared to in-person sessions, further challenging the financial viability of telehealth.
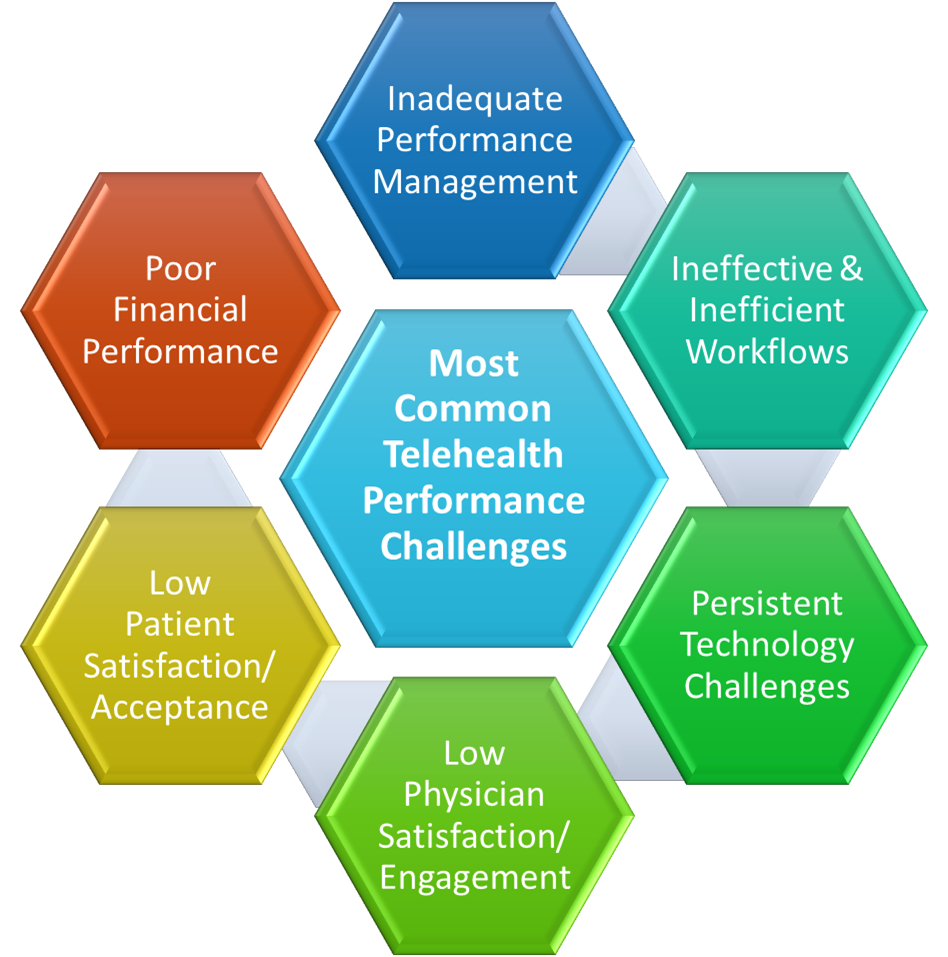


3 Common Root Causes of Mediocre Telehealth
While the characteristics of underperforming telehealth described above are quite common across a multitude of organizations, the root causes can vary widely. Many performance challenges can be explained by the change-readiness of the organization, the demographics and socio-economic status of the patient population, the experience and maturity of the leadership team, and the absence of a clinical and operational cheerleader.
For the purpose of this article, we will focus on three concrete root causes that, if turned on their head, can serve as guidance to quickly improve the performance of telehealth.
- Inadequate Performance Management
- Inefficient & Ineffective Workflows
- Persistent Technology Challenges
1. Inadequate Performance Management means that the organization’s leadership team, including the CEO, the COO, the CFO, the CMO and the CIO are pretty much unaware of the performance of their suite of telehealth services, aside from anecdotal evidence. Is the performance good? Is it improving or worsening? Without the systematic collection of key performance indicators and in the absence of setting targets for each metric, telehealth services are pretty much just limping along. As the adage goes, you can’t manage what you don’t measure, thus a common root cause for poor performance is that the leadership does not even know they have a problem.
2. Inefficient and Ineffective Workflows account for the second-most important root cause for mediocre performance. The delivery of care is ALL about workflows and poorly defined workflows are at the root of most satisfaction problems for both, clinicians and patients. E.g., very few organizations have well-defined “TeleRooming” or “Post-Visit” processes and the lack of a formal workflow leads to expensive (and frustrating) variability and missed steps or duplication of efforts.
3. Persistent Technology Challenges represents the third largest root cause of telehealth services that are not living up to the expectations. While there are some bad (or inappropriate) telehealth technologies out there, for the most part many technologies can be easily adapted to provide a smooth physician and patient experience. The secret to success here lies in proper training and support for clinicians and patients, as well as appropriately defined workflows that are optimized around the capabilities of the technology.
Improving Telehealth Service Performance
So how can an organization quickly improve its telehealth service performance — especially while Covid-19 infections are still at record levels and while we need to increase the “physical-space” capacities to make room for the vaccination administration?
The answer is quite simple: by turning the root causes above on their head and combining them with the three characteristics of poor telehealth: Create telehealth service dashboards to capture key metrics, such as volume, reimbursement, physician satisfaction, and patient satisfaction, just to name a few. Then set targets and start improving both the workflows and the technology and provide training (e.g., on “webside manners”) to clinicians to boost their confidence with this different mode of care delivery.
Or of course you could give me a call and we can chat about your organization’s unique performance challenges (Shameless Promotional Plug).
Telehealth is undoubtedly here to stay and if your organization is not serving your patients via telehealth, someone else will. The choice is yours.
Do you have performance dashboards in place? Do you periodically assess physician and patient satisfaction and act on the data? Let me know – always great to hear from you.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









I disagree with the article’s assertion that most healthcare organizations have underperformed with telehealth due to low physician satisfaction and engagement, low patient acceptance and satisfaction, and poor financial performance. It is unfair to generalize the performance of telehealth across all organizations as each organization has its own unique challenges and opportunities. The low utilization rate of telehealth during the summer of 2020 could be attributed to the reopening of some in-person healthcare services as the pandemic situation improved.
Additionally, the article does not acknowledge the positive impact of telehealth on healthcare delivery during the pandemic. Telehealth has allowed patients to access healthcare services safely, from the comfort of their homes, and has expanded access to care for those who may not have been able to receive it in-person.
While there may be some challenges with implementing telehealth, such as technological barriers and reluctance from some healthcare providers to adapt to the new model, many organizations have been successful in incorporating telehealth into their healthcare offerings. It is important to evaluate the effectiveness of telehealth on a case-by-case basis and to address any challenges faced by each individual organization.