Optimization is the science (and often art) to make the best use out of a resource. The strive for doing the right things (effectiveness) and doing things right (efficiency) leads to a continuous cycle of improvement. But when optimizing systems, which screws should you tighten or loosen? Which aspects need to be tweaked?
To guide your endeavor of improving telehealth, to optimize telehealth for getting the most value out of it, here are 5 key aspects that influence the performance of a telehealth service.
Telehealth Performance
Ultimately optimizing telehealth is about deriving the most value from the telehealth services by getting the highest return (e.g., clinical outcomes, revenue) from a minimal investment (e.g., staff and money).
The best starting point for optimization is to assess the current performance to identify which areas could benefit from improvement most. It’s like an engine with multiple cylinders – to optimize engine performance you want to make sure that all cylinders are running perfectly and you would focus your efforts on improving the performance of the weakest one. That’s the thought behind the “weakest link” expression.
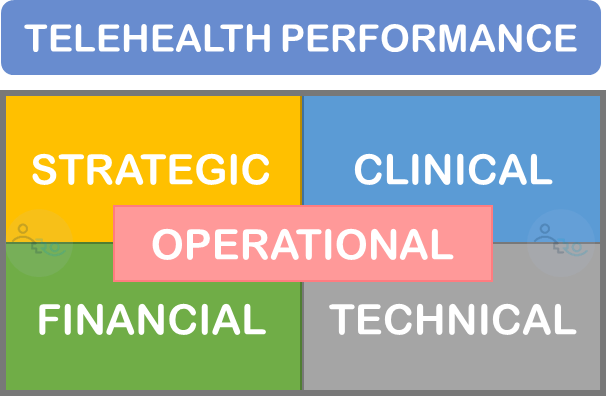
So what are the “cylinders” of the “telehealth engine”? In our evaluation of telehealth service performance we assess the following five areas:
- Strategic Alignment
- Clinical Outcomes
- Financial Value
- Technical Quality
- Operational Performance
The ultimate goal of a high performing telehealth service is that it is long-term sustainable, i.e., that the investment of money as well as personal energy by the staff yield measurable, positive returns.
Optimizing Telehealth Performance
When people first approach the assessment of telehealth performance, oftentimes the metrics are quite simple: volume and revenue. The idea of the framework above is to evaluate telehealth performance more comprehensively, more systematically.
As described above, a strong weakness in one of these 5 areas will prevent high performance in the other four, so it’s important to first identify the performance related to each of the five areas.
Strategic Alignment: A high-performing telehealth service that is sustainable must have the support and buy in of the organizational or departmental leadership. If the value generated by the service is not recognized by or not important to the organization’s leadership, the telehealth service does not have a long term future.
To optimize strategic alignment, either expand the value of the telehealth service to address strategic objectives or educate the leadership about the strategic importance of the telehealth service.
Clinical Outcomes: Ultimately everything we do in healthcare we do to improve clinical outcomes for patients. While as a healthcare delivery mechanism, telehealth cannot be held solely responsible for achieving positive clinical outcomes (that is, after all, the job of the clinicians), it is an important clinical tool if it is consciously wielded as such.
To optimize for the best clinical outcomes, explore how the telehealth service can improve the clinical diagnosis and treatment processes and improve patient engagement.
Financial Value: In our financially constrained world, a lot of the sustainability of telehealth services has to do with the financial performance. Are we getting paid? Are we getting paid as much as in-person care? Those are the questions mostly asked.
Optimization here means to ensure that only reimbursable services are scheduled and delivered. In this fast changing world of reimbursement rules (and not just toward the end of the pandemic but driven by the constant quest by the payors to lower cost), to optimize financial value means putting processes in place that catch denials early and also advise clinicians on proper coding.
Technical Quality: While security and compliance with regulations are an absolute must, they are also for the most part an expected given. Most optimization around technical performance focuses on user productivity, which is tightly coupled with the satisfaction of all types of users alike – patients, clinicians, and staff.
Optimization, first of all, focuses on taking a good hard look at whether the solutions that are in place are meeting the needs of the clinicians and patients. Oftentimes solutions were selected (by IT staff, not clinicians) because in the middle of the Covid-19 health crisis they were readily available. But now, a year later, they may no longer be the best solution for the cause. If the solution cannot or should not be changed, other optimization tactics include providing easy to access training and technical support to increase clinicians’ proficiency with the tool; and working with the solution vendors to improve the usability of their solution.
Operational Performance: Last but not least, operational metrics are the ones that are most often those that are most easily measured. Volume. No Shows. Time to appointment. Miles saved. These are all examples of operational measures and it’s first of all up to the leadership (see #1) to select the critical metrics and establish operational performance targets.
The most common optimization techniques to improve Operational Performance include the increase of internal and external marketing to raise awareness and grow volumes. In addition, a clear mapping of the operational workflows greatly accelerates root cause analyses of poor performance.
Improving Performance vs. Optimization
The Latin root of “Optimization” is “optimus” which means, simplified, means “the best”. While performance improvement is content with making things better, a mindset of optimization focuses on finding the best way to achieve outstanding results.
Optimization does not stop when metrics improve, but rather with optimization the focus is on studying the overall system and finding ways to make the processes, the training, the communication, the technology, etc. better.
Thus “improving telehealth” is a repetitive undertaking until your services are truly optimized for your organization and for your patients.
How are you approaching improving telehealth performance? Does your organization employ performance dashboards that are reviewed by designated senior leadership? Let me know!








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment