


When it comes to using technology to deliver healthcare effectively, we are in a state of widespread confusion. And this confusion is contributing to the lack of progress on the healthcare innovation front, especially on the legislative and fiscal side. For example, as one analysis revealed, no two states in the union share the same definition or regulation for telehealth.



One of the definitions of confusion is “a disorderly combination of elements with identities lost and distinctions blended”. I love that description as it paints an apt picture of the conundrum posed by the variety of terms, differing definitions, and inconsistent use of terms. How can we regulate or even simply offer any Digital Health service, if parties are not even on the same page regarding their understanding of the terms?
On the merits of clear, shared definitions
During my time at a fine academic medical center, through many “teachable” experiences, I stumbled across two aphorisms that apply here, too: “Everybody agreed until somebody wrote it down.” and “Everybody agreed until somebody defined it.”.
So, why is the definition of terms so important?
Just like “you can’t manage what you don’t measure”, you cannot manage what you can’t describe. If we don’t have a word for a concept or if we are unsure about a word’s meaning or use, we are less prone to use the word or to apply the underlying concept.
A recent article based on a radiolab show explains that the color blue did not enter modern languages until very late. In the beginning, people simply had no word for blue and poets as far back as Homer (a “wine-dark sea”) had to use comparisons to capture the essence of “blue”. Thus even though people were seeing the same thing, they could not agree on what to call it.
While we do have words for the various concepts in Digital Health, we don’t have broadly agreed-on definitions.
Now, I don’t claim that the definitions I will be proposing later on are the best ones. My hope is simply that soon everybody in the US healthcare ecosystem can agree on a single set of clear definitions and move on. In the meantime, I do urge any of you working on implementing any kind of connected health services to settle on clear definitions (you could start with the ones provided here) and to use them consistently.
Even though a “rose by any other name” might “smell as sweet”, not defining the key terms will result in confusion, which will lead to resistance to change.
As a side note – the main culprit here might actually not be the people practicing digital or connected health; more than likely the technology and solution vendors’ marketing machines are to blame for contributing to the confusion, presumably to distinguish themselves from their competition.
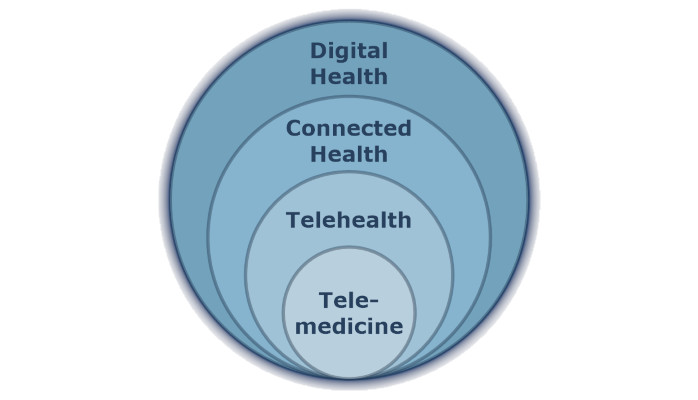
In this 3-part series, let me walk you through the three layers of a possible Digital Health Taxonomy, namely Telehealth (1st), Connected Health (2nd), and Digital Health (3rd), starting with the Telehealth Taxonomy.
A Telehealth Taxonomy
When I launched Ingenium Telehealth in 2012, I wanted to make sure that I would be using the terms in this field “correctly”, naively believing that surely the industry had agreed on a set of definitions. So I downloaded and searched about two dozen research articles on the definition of Telehealth and Telemedicine (including two or three articles comparing definitions in the research literature) and frustratedly came up empty handed. There didn’t seem to be any consensus! So, by analyzing and merging the definitions that appealed to my logical engineering mind, I settled on a my own set of definitions and created a visual to better communicate my view of the telehealth world.
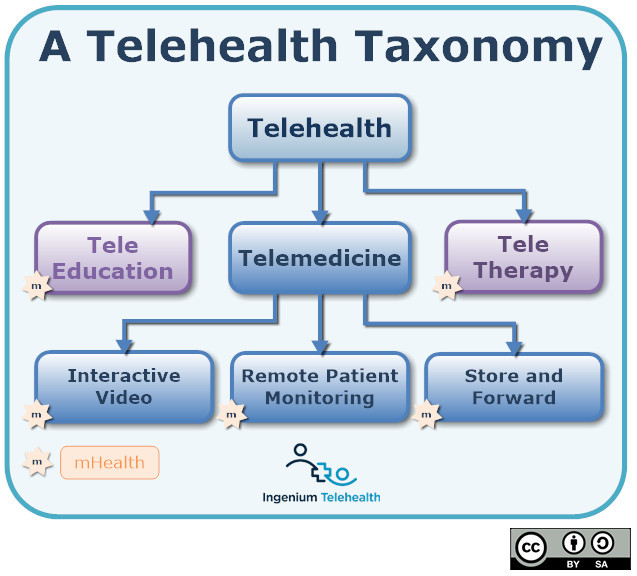


The definition I use for Telehealth is “delivering healthcare at a distance”, which includes distant health education (TeleEducation), remote treatment (TeleTherapy) and Telemedicine.
For Telemedicine, as a subset of telehealth, I used the definition of “practicing medicine at a distance” — i.e., providers examining, observing, consulting, and treating patients. Telemedicine includes:
- Interactive Patient Care: i.e., consults, visits, and exams over a secure, live audio/video connection, sometimes augmented by sharing visual information
- Remote Patient Monitoring: e.g., periodic blood pressure and weight or continuous monitoring and transmittance of activity level and heart rhythm
- Store-and-Forward: e.g., faxing EKGs, sending pictures of melanomas, and the whole domain of TeleRadiology
Simply put, Telehealth is an alternative way to deliver healthcare or to practice medicine. The only difference to our traditional care is that the patient and the physician (or other providers, educators, or therapists) are not at the same physical location. Telehealth provides physicians easy means to reach more patients outside of their clinic’s current geographic area, thus making core competitive advantages (such as expertise in a specialty area like oncology or genetic counseling) available to a larger population.
The Benefits of Telehealth
Telehealth, which is mostly about the processes and not the technology, therefore serves as an excellent strategic tool to meet the often referred triple aim of improving the quality and experience of care (a home run for telehealth), improving the health of populations (which telehealth facilitates), and reducing the per capita cost of health care (think: preventing admissions, accelerating recovery).
Telehealth can also conveniently facilitate patients’ adherence to the agreed-upon care plan, since the care team can reach and interact with patients more frequently, which dramatically improves outcomes, thereby minimizing overall healthcare cost.
And Telehealth allows caregivers, such as the patient’s family to participate more in the care even though they might not be in close proximity to their loved one, thereby further increasing care plan adherence. Family members can, for example, join an interactive telemedicine visit or see their loved one’s regular vital signs or activity level, which also provides them with an important piece of mind.
Furthermore, Telehealth is very effective for the efficient management of chronic diseases, since the tracking of the vital signs facilitates the detection of the onset of disease very early on, thereby preventing traumatic, dangerous, and expensive hospitalizations or readmissions.
Last but not least, Telehealth, in particular interactive Telemedicine, is especially appreciated by less mobile patients who either need to arrange for transportation or where transportation to the nearest clinic becomes a financial challenge due to rising gas prices and fixed incomes. The ability to receive specialty care in the familiar comfort of their home or at least their hometown clinic definitely improves health outcomes.
It is these advantages of Telehealth (delivering healthcare at a distance) and Telemedicine (practicing medicine at a distance) that really can help a healthcare organization to deliver the best care patients need, when they need it, where they want it.
In the next part I will cover the next galaxy in the Digital Health Universe: Connected Health.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.








Leave A Comment