In last week’s Telehealth Tuesday article I covered the 7 Levels of Telehealth Maturity which ranged from “chaotic” to “transformative”. In today’s article I’ll be diving deeper into the first four levels of telehealth maturity: from chaotic to emerging to coordinated to supported.
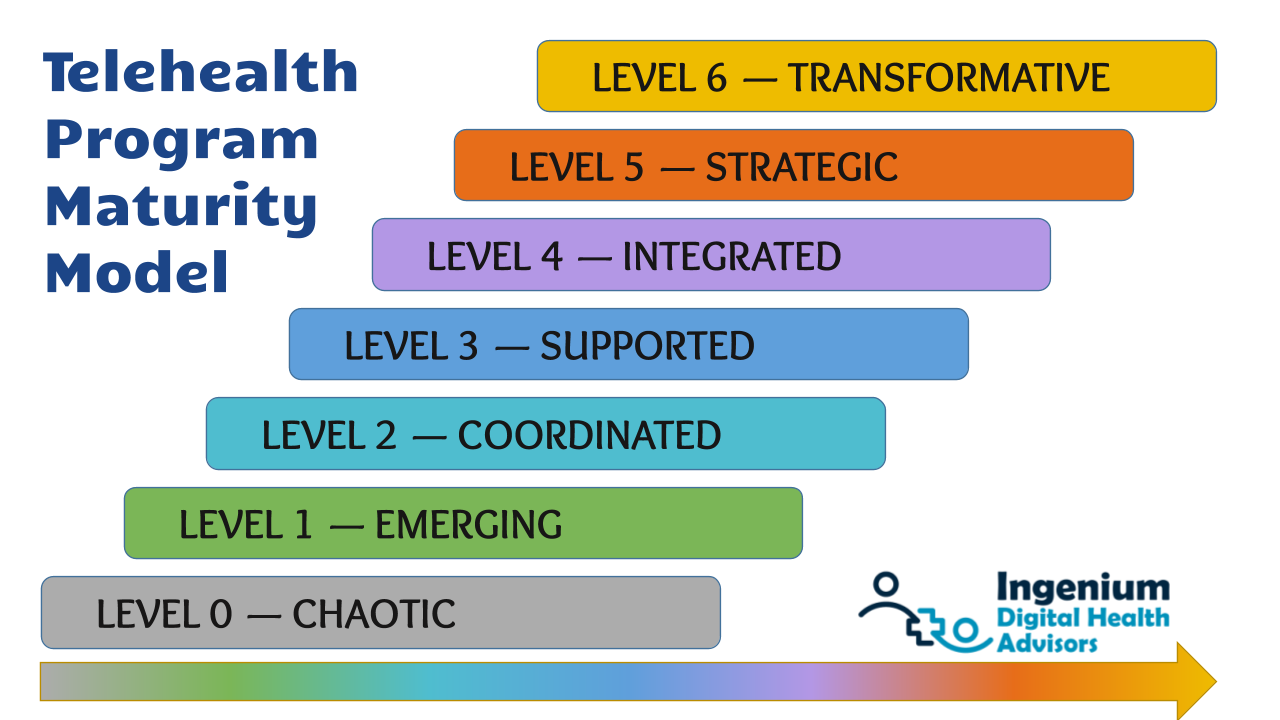


A Journey with the End in Mind
The first destination we chart for the clients we work with is the maturity level of “Supported”. At this level, the organization has fully embraced telehealth and has set resources, namely staff, aside to centrally provide support for telehealth.
This level is so important (and a good resting place before advancing to the next three levels) because it forms the foundation for a more advanced utilization of telehealth beyond the augmentation of inpatient and outpatient services. The level of “Supported” is the base from which an organization can expand into reaching the “Integrated” level, which is a significant mindshift from the historical view of telehealth.
At the supported level, the senior leadership of the organization fully embraces and values telehealth as a clinical care delivery tool and provides the necessary resources to provide sufficient operational and technical support. In addition, at this level a designated, skilled team is charged with assisting various clinical departments with the launch of new telehealth services through project management, clinical workflow design, technology selection and training.
It all starts with chaos
So where do most organizations start in telehealth? Most organizations, especially during the early months of the Covid-19 health crisis, started out at the “Chaotic” level. Each department, each service line (and even in some cases each physician) was permitted to launch telehealth in the way they thought was right or at least acceptable. Before Covid-19, enthusiastic staff, often clinicians, would secure access to telehealth technology, often with little to no coordination with IT or involvement of Finance and no coordination with other departments.
The “Chaotic” level can be good as it can create quick success due to the dedication of a clinical champion “to make it work” which can serve as positive inspiration to the rest of the organization. But the danger of launching telehealth with little to no strategic thought and no centralized, experienced support is that many services will fall short of their possibilities, because a single person, especially a clinician, can only do so much.
Now that the Covid-19 health crisis has pointed a bright spotlight onto telehealth, there is much more awareness from senior leadership, yet oftentimes no true support. The result are dismally performing telehealth service with many disillusioned clinicians that leave patient’s puzzled as to why their experience was so bad compared to their or their friends’ and family’s experience with other providers.
Telehealth Grows Up
At the next level, “Emerging”, leadership becomes aware of the strategic need for telehealth yet still does not set a central resource aside to aid in the launch and in the sustaining operation of existing and new telehealth services.
At this level of maturity, the adoption of telehealth services is accelerating and one of the first to notice (and put some coordination behind it) is the IT department, because ultimately things eventually break. While it was okay to get SaaS licenses online, working on the actual integration and configuration does require IT expertise.
At organizations with an “Emerging” maturity level, leadership awareness and endorsement (though not support) is present, IT is much more involved and some attention is paid to the financial performance of the services.
The last step toward the final destination is “Coordinated”. Here, the different telehealth services across the organization are coordinating their efforts. At times an unofficial person, sometimes from billing, sometimes from IT and sometimes from informatics, emerges as the knowledgeable resource, though the position is not appropriately funded. Success is still based on the heroic efforts of a few individuals.



Are we there yet?
Without leadership’s involvement and support, things don’t really move beyond the coordinated level. Since launching telehealth successfully requires a multi-disciplinary approach. This includes leveraging technical support, billing knowledge, compliance, project management, training, and clinical workflow design. Without it, progress is hindered until dedicated resources are allocated to supporting the launch and operations of telehealth.
In order to reach the “Supported” level, leadership truly needs to “wrap their mind around” that telehealth is there to stay and has established itself as a viable, long-term care delivery mechanism, akin to in-person outpatient visits and inpatient visits.
All of the health systems we work with want to reach the Supported level and are primarily interested in the development of a telehealth program strategy and a telehealth program business plan that looks more systematically at the opportunities ahead.
Look for next week’s article for an exploration on the Levels 4, 5, and 6 to literally take telehealth maturity (and its value to the clinicians and the patients) to the next level.
Where would you put your organization’s maturity level? Are you fully at level 3? When do you think you’ll reach level 4 (“Integrated”) or level 5 (“Strategic”)?








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment