Digital Health is quite a broad term that it is challenging for many healthcare leaders to put their arms around the totality of it all, when trying to decide where to focus their attention (and investments of time, money, and people).
I’d like to remind us that technology primarily exists to serve us, to make our lives easier or safer — or both. When looking at Digital Health it is thus important to understand how that technology is supposed to help us.
A Definition
Our healthcare system exists to help people to get well and to stay well. To accomplish this, clinicians assess the patient’s condition, decide on how to learn more, and treat the patient by fixing the problem and healing the patient.
At its core, each hospital, health system, or clinic manages three basic sets of activities
- Care Decisions – for diagnosis and treatment plans
- Care Delivery – assessments (exams, consults) and treatment (procedures, therapy)
- Healthcare Logistics – e.g., scheduling, ordering, billing, hiring, etc.
My definition of Digital Health therefore is simple:
Digital Health is the use of Digital Technologies
to improve the Efficiency and Efficacy
of Care Decisions, Care Delivery, and
Ancillary Healthcare Processes.
While efficacy is about doing the right things, efficiency is about doing things right. And digital technologies can help us to accomplish both.
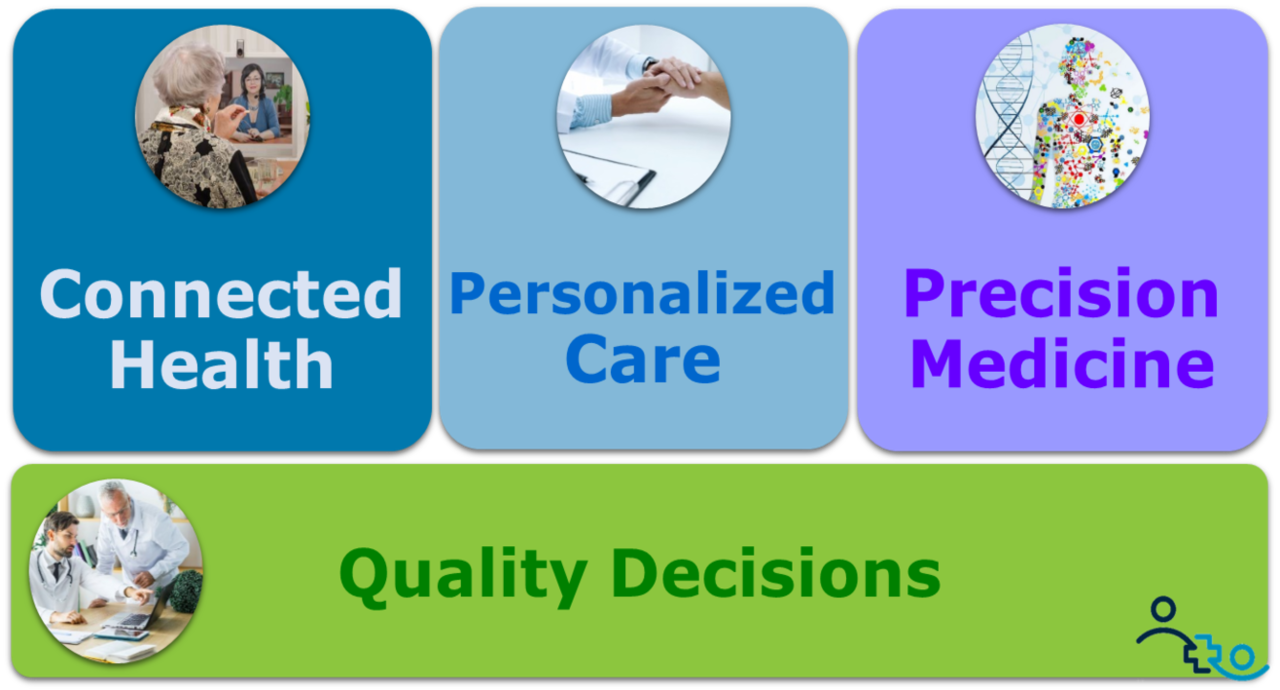
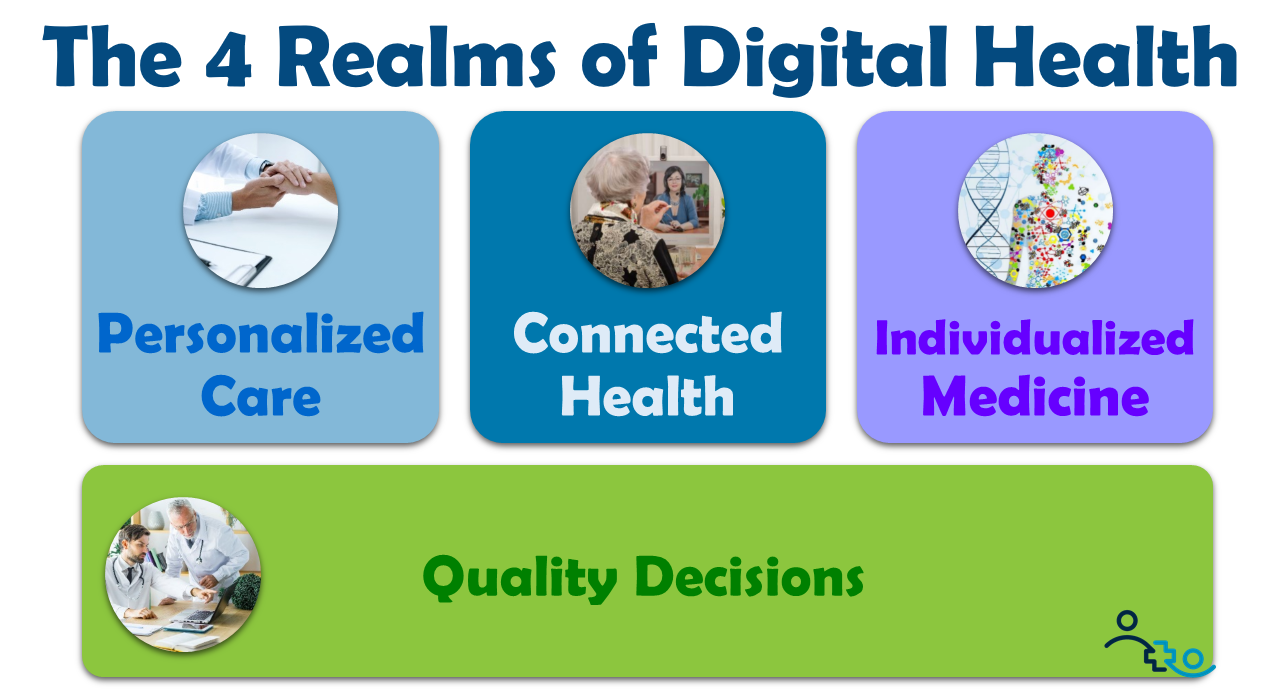
The Four Realms of Digital Health
In the avalanche of digital health that’s barreling toward us, I see four different distinct areas of innovation that all need to be addressed and managed in parallel:
- Personalized Care: Offering a highly personalized, exceptional care experiences
- Connected Health: Empowering patients to get well and stay well anywhere, any time
- Individualized Medicine: Tailoring medical treatment to a patient’s unique characteristics
- Quality Decisions: Empowering physicians, patients and administrators to make better decisions


Investing in Digital Health
So why would an organization need to spend resources on each of those four realms?
Healthcare consumers’ expectations also create the notion that scheduling, receiving and paying for healthcare should be as easy as paying a friend via Venmo, ordering a book from Amazon, or renting a movie from Netflix. One key aspect of convenience here is Connected Care with its digitization of healthcare information and helping to transcend geographic boundaries through virtual and tele-technologies.
A Personalized Care approach is necessary as patients have evolved into healthcare consumers and have much higher expectations from their care experience. This starts with the scheduling of appointments, continues with the check-in process and culminates in the personalized approach used by the clinician. Digital Health solutions, such as healthcare CRM (customer relationship management) systems and optimized EMRs can greatly support the physician and allied health staff to provide a great service experience.
With the increasing insights into how unique humans are in their health, it also behooves healthcare providers to at a minimum provide access to early Precision Medicine services, e.g., such as (tele) genetic counseling. As solutions become more accessible and financially feasible, they can be integrated into your current care decision and care delivery processes.
Finally — and most importantly — the realm of enabling High-Quality Decisions. Healthcare’s most valuable asset is undoubtedly the clinical data. Without good access to good data, physicians cannot make decisions about diagnosis or treatment. The same goes for patients who, as the current debate goes, cannot make good financial decisions regarding their care, because there is no good data.
Looking Ahead
Over the next weeks I’ll dive deeper into each of those four realms because the better you understand the implications of each, the better informed decisions you can make where to invest your and your organization’s resources into digital health innovation.








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.







Leave A Comment