A Guide for Leaders in Healthcare
In the week leading up to Christmas 2021 it is now all but certain that over the holidays and well into January, the Omicron variant will once again put a strain on our healthcare delivery system. With just 4% of new cases being identified as the Omicron variant last week, this week already 75% of all new cases are Omicron.
Especially in healthcare, these past months have been extremely exhausting from the Delta variant in late summer to vaccine mandates in the fall and now Omicron just in time for the winter season. I’m sincerely hoping that we’ll get a break from Covid in the spring.
While over the past 21 months Telehealth has certainly been on the mind of healthcare’s leaders, it has taken somewhat of a backseat especially over the past months. While those organizations who had telehealth in place before the pandemic have continued to stabilize and build out their telehealth services, those who were quickly pushed into telehealth also retreated almost as quickly out of it.
Over the past months many leaders, especially in the health center and rural clinic world, however, have realized that telehealth is here to stay (and more and more patients are demanding it) and actually a quite helpful tool.
If what was needed to push telehealth to the next level for your organization, Omicron may just provide that burning platform. In order to successfully and swiftly combat Omicron in your community while keeping the doors open for Covid and non-Covid patients alike, here’s a battle plan.
A 9-Step Telehealth Battle Plan for Omicron
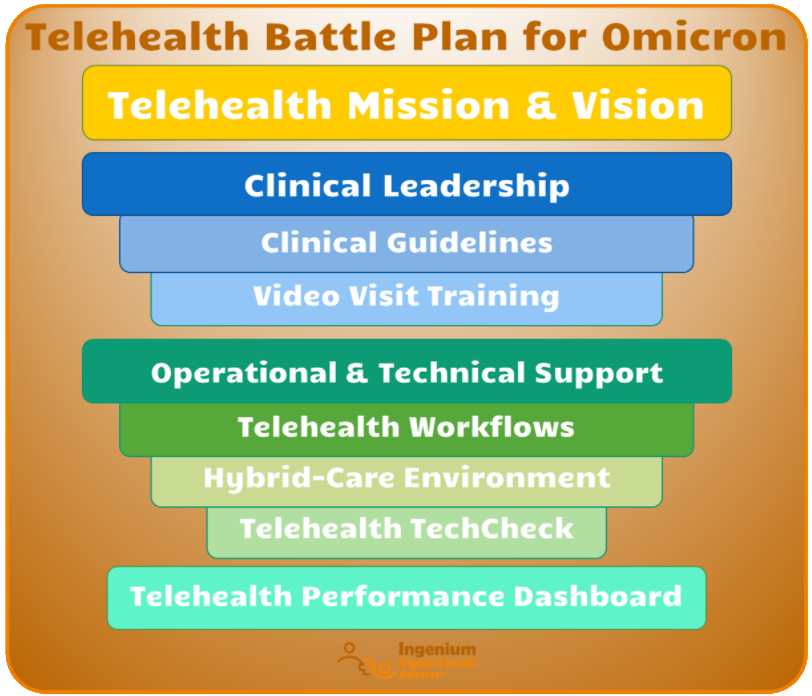


A good plan is half the battle
Exclusive Offer for Healthcare Leaders
Join Christian for a 60-minute value-packed workshop with Q&A
this Thursday, December 23 at 12 PM Eastern.
Forward the link to share this workshop with your peers and colleagues!








To receive articles like these in your Inbox every week, you can subscribe to Christian’s Telehealth Tuesday Newsletter.
Christian Milaster and his team optimize Telehealth Services for health systems and physician practices. Christian is the Founder and President of Ingenium Digital Health Advisors where he and his expert consortium partner with healthcare leaders to enable the delivery of extraordinary care.
Contact Christian by phone or text at 657-464-3648, via email, or video chat.









Leave A Comment